Cataract is the leading cause of avoidable blindness in the world. According to a 2010 assessment, cataract is responsible for 51% of world blindness, representing about 20 million people. Although cataracts can be surgically removed, in many countries barriers prevent patient access to surgery.
AT A GLANCE
• Intratunnel phacofracture is a nucleus management technique, in which the lens nucleus is broken inside a sub−6-mm sclerocorneal tunnel and removed.
• The nucleus removal steps take place inside the corneoscleral tunnel, in contrast with other nucleotomy techniques in which this maneuvering takes place inside the anterior chamber.
Manual small-incision cataract surgery (MSICS) and phacoemulsification are the most popular methods of cataract extraction today. The former is significantly faster, less expensive, and less technology-dependent than phacoemulsification and has been extensively practiced in developing countries such as India. However, the drawback of most commonly practiced MSICS techniques—Blumenthal, viscoexpression, irrigating wire vectis, and fish-hook needle—is that they all require a large incision of 7 to 9 mm, which leads to induced astigmatism.
I posed the following question to myself: What if the nucleus could be removed though a sub−6-mm incision at the appropriate site? After some research, I came to the conclusion that this would result in approximately the same astigmatism induction as a 3.2-mm phaco incision.1-4 From there, I devised the intratunnel phacofracture technique,5 in which the lens nucleus is broken inside a sub−6-mm sclerocorneal tunnel incision and removed. The nucleus removal steps take place inside the corneoscleral tunnel, in contrast with other nucleotomy techniques in which this maneuvering takes place inside the anterior chamber. This article provides a step-by-step description of my original technique, with an accompanying video demonstration available at http://bit.ly/singh0516.
SURGICAL PLANNING AND STEPS
Planning. The incision site is chosen according to keratometry values (K1 and K2). If the difference between K1 and K2 is 1.00 D or less, the superotemporal quadrant in a right eye or the superonasal quadrant in a left eye should be chosen (Figure 1A). If the difference is greater than 1.00 D, then the incision should be made on the steeper axis. If K1 is steeper than K2, then a superior incision should be made (Figure 1B), and, if the reverse is true, then a temporal incision should be made (Figure 1C).
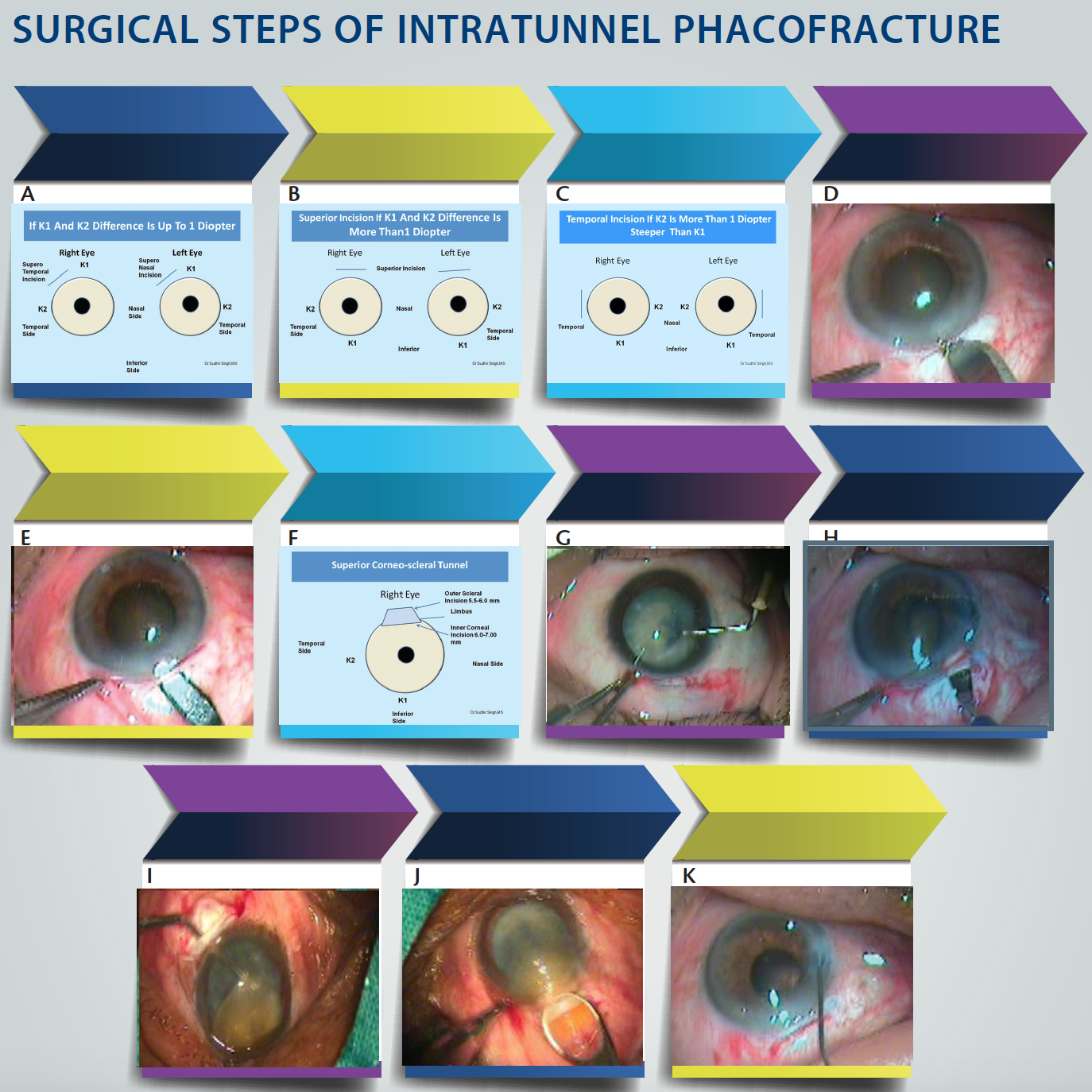
Figure 1. If the difference between K1 and K2 is less than 1.00 D, then a superotemporal incision is used for a right eye and a superonasal incision for a left eye (A). If K1 is more than 1.00 D greater than K2, then a superior incision is used in both right and left eyes (B). If K2 is more than 1.00 D greater than K1, then a temporal incision is used in both right and left eyes (C). Fornix-based conjuctival flap, cautery, and partial scleral groove creation (D). Corneoscleral tunnel creation (E). Sclerocorneal tunnel dimensions in superior quadrant (F). Capsular staining and capsulorrhexis creation with needle capsulotome (G). Tunnel enlargement with a 5-mm keratotome is followed by enlargement of the internal incision with a 2.8-mm keratome (H). Nucleus rotation and prolapse into anterior chamber (I). Intratunnel phacofracture using Lewis lens loop (J). Irrigation and aspiration, IOL implantation, and wound sealing with hydration, followed by conjunctival flap repositioning (K).
Step No. 1. MSICS procedures including the intratunnel phacofracture technique can be performed under peribulbar or topical anesthesia. The skin of the eyelids, lid margins, and around the eye should be cleaned with 10% povidone-iodine solution. The drape is applied, and a wire speculum is placed. The cul de sac is thoroughly washed with Ringer lactate solution or balanced saline solution.
Step No. 2. A 4-0 silk superior rectus bridle suture is placed beneath the tendon of the superior rectus muscle. This is helpful for positioning the eye after local anesthesia. A superior rectus bridle suture is not used when surgery is planned under topical anesthesia.
Step No. 3. A fornix-based conjunctival flap at the limbus with a chord length of approximately 6.5 mm is made. After careful dissection of Tenon capsule, light cautery is applied (Figure 1D). A 6-mm scleral frown incision, 1.5 mm from the limbus, is made with a No. 15 Bard Parker blade (Figure 1E). A funnel-shaped sclerocorneal tunnel incision is created with a steel crescent knife. One sideport is made 90º on either side of the scleral tunnel with a 15º knife, temporally in a right eye and nasally in a left eye.
Step No. 4. With a 2.8-mm keratome, the anterior chamber is entered 1.5 mm into the clear cornea with the help of a 3.2-mm keratome (Figure 1F). A hydroxypropylmethylcellulose 2% OVD is injected into the anterior chamber.
Step No. 5. A central curvilinear capsulorrhexis is made with the help of a 26-gauge needle capsulotome. If the red reflex is poor, the capsule is stained with trypan blue dye under an air bubble. Then the OVD is injected and the capsulorrhexis is made. The size of the capsulorrhexis, which depends on the size of the nucleus, can vary from 5.5 to 7.5 mm (Figure 1G). If the nucleus size is anticipated to be large, then two relaxing incisions are made at the margins of the capsulorrhexis. The capsulorrhexis can also be made using capsulorrhexis forceps.
Step No. 6. Hydrodissection is performed with a 26-gauge cannula on a 2-cc syringe filled with irrigating fluid.
Step No. 7. The internal dimension of the tunnel incision is enlarged sideways to 7 mm with a 5.1-mm keratome (Figure 1H). The anterior chamber is then re-formed with OVD, and the nucleus is rotated within the capsule using a Sinskey hook.
Step No. 8. The nucleus is prolapsed into the anterior chamber using the Sinskey hook. The device then is used to retract the capsulorrhexis, engage the equator of the nucleus, and lever one pole of the nucleus out of the capsular bag. The rest of the nucleus is then rotated into the anterior chamber. If the nucleus is too large, two or three relaxing incisions can be made at equidistance at the capsulorrhexis margins (Figure 1I).
Step No. 9. (Up to this point, all the above-mentioned steps are the same as they would be in other MSICS techniques. Step No. 9 is when intratunnel phacofracture diverges from other phacofracture techniques.) OVD is placed between the cornea and the superior surface of the nucleus to protect the endothelium and between the nucleus and iris to keep these tissues separated. The nucleus is rotated within the capsule using a Sinskey hook. The globe is stabilized with toothed forceps, and a small Lewis lens loop (AA 1915; Appasamy Associates) is introduced through the tunnel and positioned between the iris and the nucleus. The nucleus is engaged in the lens loop and slowly withdrawn from the anterior chamber while the posterior lip of the tunnel is depressed.
Step No. 10. Once the nucleus is engaged in the tunnel, the Lewis loop is pulled posteriorly and upward, causing a portion of the nucleus to break and initiating removal; another portion remains engaged in the tunnel. With more OVD, the engaged portion of the nucleus is pushed back into the anterior chamber and rotated so that its longitudinal axis coincides with the longitudinal axis of the tunnel.
Step No. 11. Again OVD is placed between the cornea and superior surface of the nucleus and between the nucleus and iris. The lens loop is introduced through the tunnel and positioned between the iris and the remaining part of the nucleus, which is then engaged in the lens loop and slowly withdrawn from the anterior chamber while the posterior lip of the tunnel is depressed.
Most of the time, at this point, the remaining part of the nucleus comes out. If it breaks down further, then any remaining part is again pushed into the anterior chamber with the help of OVD, and the previous steps are repeated until it comes out (Figure 1J).
Step No. 12. Cortical cleanup is done directly with a 23-gauge Simcoe I/A cannula. The anterior chamber is re-formed with OVD (Figure 1K).
Step No. 13. A one-piece PMMA IOL with an optic size of 5.5 to 6 mm and overall length of 12.5 mm is implanted into the capsular bag. The anterior chamber is washed out thoroughly with the Simcoe cannula using Ringer lactate solution (Figure 1K).
Step No. 14. The conjunctival flap is repositioned and cauterized at the edges. The main and sideport incisions are sealed with stromal hydration using a 26-gauge cannula. A 0.5-cc subconjuctival injection of gentamycin with dexamethasone is given, and the eye is padded and patched.
CONCLUSION
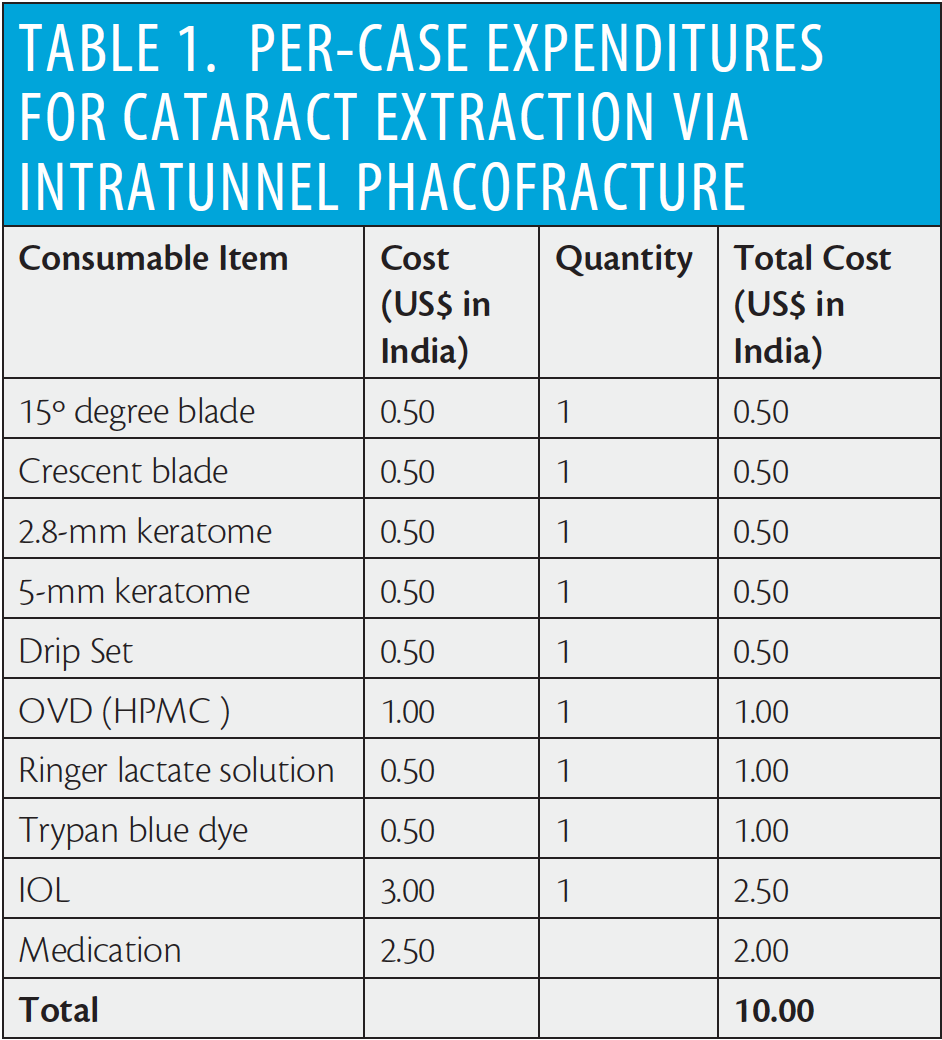
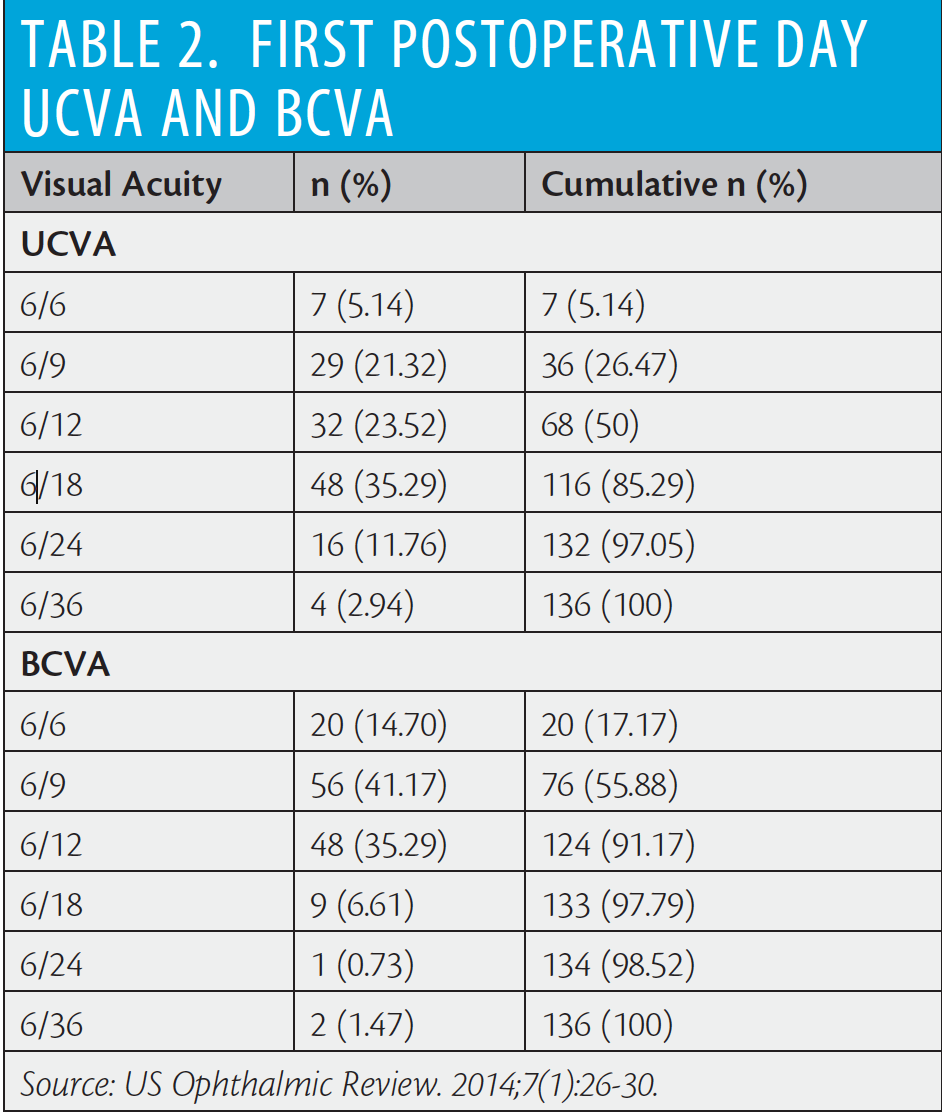
The intratunnel phacofracture nucleus management technique is simple, inexpensive, and reproducible. Per-case consumable expenditure for cataract extraction using this technique is shown in Table 1, and postoperative day 1 visual outcomes in a series of patients are presented in Table 2. In short, the mean UCVA and BCVA on the first postoperative day in this series of patients were logMAR 0.367 (Snellen equivalent 20/46) and logMAR 0.226 (Snellen equivalent 20/33), respectively. No serious peri- or postoperative complications were encountered, and all types of cataracts were successfully removed.5
1. Oshika T, Nagahara K, Yaguchi S, et al. Three year prospective randomized evaluation of intraocular lens implantation through 3.2 and 5.5 mm incisions. J Cataract Refract Surg. 1998;24:509-514.
2. Gokhale NS, Sawhney S. Reduction in astigmatism in manual small incision cataract surgery through change of incision site. Indian J Ophthalmol. 2005;53:201-203
3. George R, Rapauliha P, Sripriya AV, Rajesh PS, Vahan PV, Praveen S. Comparision of endothelial cell loss and surgically induced astigmatism following conventional extracapsular cataract surgery, manual small incision surgery and phacoemulsification. Ophthalmic Epidemiol. 2005;12(5):293-297.
4. Gogate PM, Kulkarni SR, Krishnaiah S, et al. Safety and efficacy of phacoemulsification compared with manual small-incision cataract surgery by a randomized controlled clinical trial: six-week results. Ophthalmology. 2005;112(5):869-874.
5. Singh S. First postoperative day visual outcome following 6 mm manual small incision cataract surgery using intratunnel phacofracture technique. US Ophthalmic Review. 2014;7(1):26-30.
Sudhir Singh, MS
• Senior Consultant and Head of Department of Ophthalmology, J.W. Global Hospital and Research Centre, Mount Abu, Rajasthan, India
• drsudhirsingh@gmail.com
• Financial interest: None acknowledged