
After years of eye mission trips to Southern Africa, I have learned numerous valuable lessons that I have been able to apply to my daily practice of ophthalmology. The most important lesson I learned for myself and for my practice in the United Kingdom is the value of a team, and the greatest thing I learned to appreciate is the difference one can make in a patient’s life. Allow me to explain my journey in practicing ophthalmology in developing countries, where I gained noticeable personal benefits including improvements in my own surgical abilities and in my approach to high-volume, high-quality cataract surgery. I also gained other invaluable experiences in research, business planning and management, and teaching.
My first time in Malawi, a landlocked country in southeastern Africa, I needed the first 2 weeks just to get settled in. There was something about the mosquitoes, the threat of malaria, the hyenas at the top of the garden howling at night, and the children staring at me all the time whispering “mzungu” (a Bantu language term for European) that took time to get used to. Other initial challenges included the daily power outages, the lack of phone reception, and the need for trips to a town 2 hours’ drive away for Internet access.
To be honest, in a rural, low-income, developing-world setting, the problems of the developed world soon fade into insignificance. It is a simple yet liberating freedom. It allows mindfulness and presence to focus on the tasks at hand: life and work in a rural hospital in one of the poorest countries in sub-Saharan Africa, if not the world.
THE BURDEN OF DISEASE
In the region of Malawi that I and one other ophthalmologist served, the population was 4 million people. Of these, an estimated 40,000 are bilaterally blind (visual acuity <3/60), and four times that number are severely vision impaired. Half of the blindness is due to cataract.
As I stared across the villages in the Linthipe valley toward the Dedza mountains and Lake Malawi beyond, I realized the colossal size of this burden. In this region where there is one ophthalmologist per 2 million people, the backlog of cataract patients alone, per surgeon, is 10,000 blind and 40,000 vision-impaired. Glaucoma, trachoma, and childhood blindness are significant problems as well. This is an area of extreme poverty, where more than 90% of the people are subsistence farmers and do not have the means to come to a hospital. It is up to the practitioners to go out and find them, and we are only a small but dedicated team of 30 staff.
FOCUS AND TAKE CARE
There is an African proverb: How do you eat an elephant? In small pieces, one bite at a time, with a lot of help from your friends.
I like to think that proverb holds weight in mission eye work. Yes, it is true that you cannot save the world. You cannot save a continent, or even a country. You cannot tackle the 20,000 to 50,000 cataract surgeries that each ophthalmologist in Africa would have to perform right now to clear the backlog. You can, however, serve the person in front of you. You can serve his or her family. You can serve his or her community. You can do this by playing a small but crucial part in a huge team effort.
It is important in mission work to keep yourself safe—especially considering the malaria and hyenas. It is also important not to become too heavily burdened by the scale of need, and to take care of yourself as well as the long lines of patients you serve. As I have learned to take time for myself during heavy workloads in Malawi, I have applied the same lesson to work in the UK National Health Service (NHS). There will always be patients, but there will not always be time for a cup of tea; so if you get the chance, take it.
After my first 2-month trip to a mission eye hospital in rural Malawi, I returned to the United Kingdom in a state of reverse culture shock. I simply could not believe that I had experienced something so rewarding and life-changing. Yet nothing at home had changed, and my colleagues could not grasp the impact that what I had been through had on me.
After my second 2-month trip, I returned with a plan: I would spend at least 4 years full-time in Malawi. Having the privilege to operate on someone who has had white cataracts with light-perception visual acuity for the past 7 years, and who can see the next day with a UCVA of 6/12 or 6/9, is the kind of work you never tire of. It is simply, innately, too rewarding.
SURGERY
Ophthalmic surgeons like to perform microsurgery—the more the merrier. During my 4 years in Malawi, I performed more than 7,000 cataract operations and 250 trabeculectomies (Figure 1). The vast majority of these were fully audited for outcomes (vision, complications, and IOP). I cannot overstate how beneficial it has been to continuously record and audit the outcomes of cataract and trabeculectomy surgeries. It has allowed me as a surgeon to review and refine my techniques and subsequently to improve my patients’ outcomes.
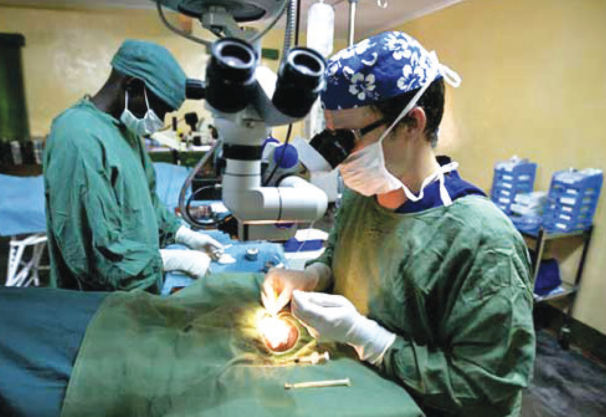
Figure 1. The author operating in Nkhoma Mission Hospital.
During my years in Malawi, and upon my return to practice in the United Kingdom, there is no doubt that my abilities as a surgeon improved. I had an excellent surgical teacher in Malawi, and I became proficient under his kind tutelage. It was, however, the subsequent demands of the long daily surgery lists, with complex and advanced cases, that helped me to develop the intuitive and adaptive abilities to deal with challenging surgical situations.
My approach to high-volume surgery has changed as a result of my experience. I see every single patient as uniquely important, every operation as different, and every step as crucial. The only way to be a fast surgeon is not to try to be fast, but instead to focus on getting every single step right and being exceedingly efficient. Paperwork should be prepared in advance as much as possible; there is no time to waste between cases. Time in the operating room must be time on the task at hand. I learned this lesson daily in Malawi when there were lines of 20, 30, even one day more than 50 individuals waiting patiently in the waiting area for cataract surgery (Figure 2). You just get on with it; but you focus on quality, not quantity. The instant you rush or cut too sharp a corner, there will be a complication that will take much longer to deal with adequately.

Figure 2. Patients waiting for cataract surgery in Nkhoma.


Figure 3. A patient before (A) and after (B) MSICS.
Over the years, I have learned and mastered a cataract surgery technique appropriate for mature cataracts (Figure 3). I would never have learned such a technique in the United Kingdom. There is nothing small about the scleral incision and tunnel in manual small-incision cataract surgery (MSICS). Yes, the 7- to 8-mm incision is smaller than the conventional limbal incision used in sutured extracapsular cataract extraction (ECCE)—but not by much. Some have thus taken to calling the procedure sutureless ECCE, or scleral tunnel cataract surgery. A version of the procedure can be viewed in the video below.
I have subsequently used the MSICS procedure a number of times in the United Kingdom for patients with very mature cataracts. The results have been impressive: for instance, in one case, improvement from light perception preoperative to 6/9 postoperative UCVA. The technique results in less postoperative astigmatism and fewer suture-related complications compared with limbal sutured ECCE. The outcomes of SICS are comparable with those of phacoemulsification.1-4
TEAMWORK, PARTNERSHIPS, AND TEACHING
You cannot perform high-volume cataract surgery alone. The only way you can perform high-volume, high-quality surgery is as part of a team, and a very well-motivated team at that. My time in Malawi, along with a few cross-border trips into northern Mozambique, solidified my understanding and appreciation that the highest quality and volume of surgery happens only with, and within, a good team. The Nkhoma Mission Hospital eye department team was outstanding and incredibly motivated, and it was humbling to work with them (Figure 4).

Figure 4. The Nkhoma Eye Department team, 2010.
I have traveled extensively around Southern Africa; however, for most of the past decade I have been returning to one or two eye hospitals in Malawi. It is by returning to the same place over the years, and living in the same region for 4 full years, and committing to individual medical units that one builds real and long-lasting relationships and partnerships.
The value of building long-lasting partnerships was a valuable lesson to learn. We partnered with other government and mission health care teams of eye care professionals to work together. We partnered with donors and nongovernmental organizations (NGOs) for help with fund-raising. I sat on the National Committee for Prevention of Blindness for advocacy, and I partnered with national and regional teaching institutions.
Clinical experience in Malawi was incredibly rich and varied. There is tropical pathology that I simply would not see in my clinic in an urban UK setting. Furthermore, I encountered advanced and end-stage pathology that is otherwise generally seen only in textbooks. With the variety of clinical presentations come long lines of patients in the clinic, so it was important to have the clinical diagnostic and management acumen to safely and efficiently work through a list of 50 or 60 patients in clinic in the morning, as the afternoon will follow with a list of 20 or 30 people needing surgery.
Despite having huge clinical and surgical service-provision duties, it was also important for me to commit to the teaching and surgical training of ophthalmology residents and nonphysician cataract surgeons. I developed valuable links with the faculties of the Malawi College of Medicine and the Malawi College of Health Sciences, and I also participated in a local program of teaching within the mission hospital. I have brought this ongoing passion and commitment to teaching and learning back to the United Kingdom, not only undertaking regular clinical teaching sessions but also completing a masters degree in surgical education.
AVAILABILITY AND FLEXIBILITY ALWAYS PAY BACK
One of the great lessons I learned in Malawi was to embrace a work ethic of being flexible and available. Every single day in the village of Nkhoma, I would hope to get to bed after a normal, straightforward day during which nothing out of the ordinary had happened; that day never came. The ability I developed there of being a team player and of being available and flexible has been beneficial since my return to the United Kingdom.
Being available and flexible always pays back. When I was called by a veterinarian at the Lilongwe Wildlife Centre to come into town on a Thursday afternoon to examine a one-eyed pseudophakic lioness named Bella, I made sure I was available. Happily, I found that the patient was anesthetized for the examination (Figure 5).

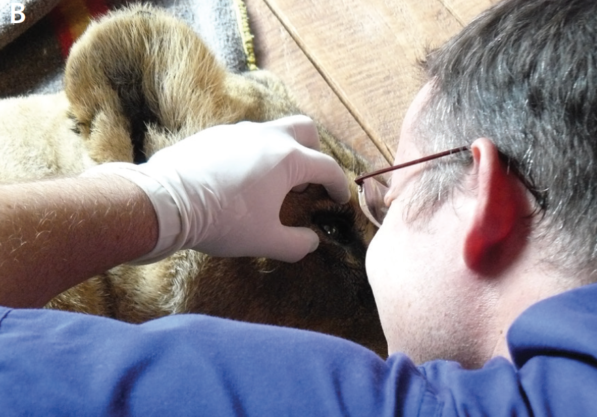
Figure 5. Bella, the pseudophakic lioness (A,B).
THE PEOPLE
The warm, kind people of Malawi have proudly earned the country the name of the “Warm Heart of Africa.” The work there always reminds me of the global connectivity of things. Kind donors from all around the world raise funds for NGOs. The NGO staff tirelessly facilitates the eye work of the teams and partner institutions on the ground, enabling them to serve the poorest of patients, who might otherwise be blind. I have developed wonderful global professional links and relationships over the years. Meanwhile, back in the United Kingdom, I respect the fact that there are people from all over the world who contribute to the NHS. One of the most enlightening benefits from my time in Malawi was developing a deep appreciation of the people and facilities of the NHS.
Most of all, I have learned an understanding of humanitarianism. I will never forget my encounter with Mr. Luka, from Dedza, one of the first bilaterally blind patients in whom I operated both cataracts. There was nothing more rewarding than seeing Mr. Luka after his second cataract operation. After two 10-minute operations over the course of 2 days, he could return to his village and see his five grandchildren for the first time. Until then, and for the past 7 years, he had known them only by the sounds of their voices. Knowing that was incredibly humbling and rewarding. When I saw him before his return home, his smile had a profound and long-lasting effect on me.
1. Ruit S, Tabin G, Chang D, et al. A prospective randomized clinical trial of phacoemulsification vs manual sutureless small-incision extracapsular cataract surgery in Nepal. Am J Ophthalmol. 2007;143(1):32-38.
2. Gogate P, Deshpande M, Nirmalan PK. Why do phacoemulsification? Manual small-incision cataract surgery is almost as effective, but less expensive. Ophthalmology. 2007;114(5):965-968.
3. Haripriya A, Chang DF, Reena M, et al. Complication rates of phacoemulsification and manual small-incision cataract surgery at Aravind Eye Hospital. J Cataract Refract Surg. 2012;38(8):1360-1369.
4. Riaz Y, de Silva SR, Evans JR. Manual small incision cataract surgery (MSICS) with posterior chamber intraocular lens versus phacoemulsification with posterior chamber intraocular lens for age-related cataract. Cochrane Database Syst Rev. 2013;10:CD008813.



