
We are now well into the 21st century. Many of us thought that, by this time, world blindness would have been adequately addressed. Although world blindness has decreased since the 1990s despite an aging world population, the reality is that 285 million people around the world are still visually impaired, 39 million of whom are blind.1
Great work has been done in reducing infectious diseases, specifically onchocerciasis and trachoma, and governmental initiatives mostly in association with nongovernmental organizations (NGOs), charities, and private groups have reduced world blindness by improving awareness, education, screening, and access to necessary treatments. However, refractive error continues to account for a staggering 43% of the world’s visual impairment, cataract 33%, and glaucoma 2%.1 Further, approximately 90% of the visually impaired live in developing countries,1 a consequence of economics affecting resources. As a result, the elimination of blindness will require several efforts, among them:
Allotment of considerable funds to identify and treat conditions;
Implementation of public health systems; and
Education of personnel.
LET’S DO MORE
Correcting refractive error through the provision of glasses is theoretically the simplest and least expensive option to reduce visual impairment worldwide. Optometrists from groups such as Vision Aid Overseas volunteer their time performing refraction and dispensing glasses in developing countries. Another unique and successful model was developed by Sean Walls, an optical technician in Glasgow, United Kingdom. With his charity Sight Aid International, Sean has established centers in Kenya and Malawi that distribute glasses at no charge, in particular to children.2 I hope to work with him to establish another center in Zanzibar in the future.
Although such work is crucial in combating world blindness and visual impairment, I believe we can do more to fund major initiatives and programs that could have considerably larger impacts on eliminating blindness. For starters, public health and education programs can increase awareness of blindness prevention activities in underserved populations. At the same time, training programs to improve the diagnostic and surgical skills of ophthalmologists and allied personnel in developing countries can provide sustainable long-term success. Projects such as Orbis, the brainchild of my mentor David Paton, MD, have for several decades positively influenced the training of doctors worldwide. In turn, Orbis has had a long-term impact on patients in countries such as Bangladesh, Cameroon, China, Ethiopia, Ghana, India, Latin America, the Caribbean, Nepal, South Africa, and Vietnam.
Despite these outreach efforts, there are few ophthalmologists practicing full-time in developing countries. The ratio across 23 of these is a staggering one ophthalmologist to every 1 to 2 million people. On the other hand, of the more than 200,000 ophthalmologists worldwide, half practice in only six countries: China, United States, Russia, Japan, Brazil, and India.3 To be more effective in treating world blindness, efficient care delivery programs are required.
Luckily, excellent work is under way, with projects for instance promoting rapid manual small-incision cataract surgery and information exchange to improve mechanisms for delivery by visionaries such as Sanduk Ruit, MD, and Geoffrey Tabin, MD, both of the Himalayan Cataract Project . In India, large organizations such as the Aravind Eye Care System and the L.V. Prasad Eye Institute have evolved considerably over the past 3 to 4 decades and have had phenomenal impact within the country. Both serve as success stories of what can be achieved thanks to the visionaries Govindappa Venkataswamy, MD, and Gullapalli N. Rao, MD, FACS, FRCS, DSc, DMed, respectively. The same can be achieved in other developing countries, and perhaps more rapidly, through replication and knowledge transfer.
THE IMPORTANCE OF INDIVIDUAL EFFORTS
Much can also be accomplished on a smaller scale through the efforts of individuals. Every effort, no matter how small, makes a difference in combating world blindness. I often meet colleagues who make regular contributions to reducing blindness by undertaking mission trips to developing countries. In speaking with them, I am often struck by their demonstrable joy when they discuss their trips and anecdotes. Working in developing countries, often in rural settings, and recalibrating in terms of evaluation and provision of care is challenging but at the same time fun.
Over the past 20-plus years, I have regularly visited Comprehensive Community Based Rehabilitation in Tanzania (CCBRT), teaching and performing complex corneal transplants. I am indebted to the generosity of Visionshare, an organization that has provided graft tissue gratis for the past 2 decades, and to the hospitality of ophthalmic colleagues and administrators at CCBRT (Figures 1 and 2).

Figure 1. The author (center) with Kazim Dhalla, MD (right), and head nurse at CCBRT (left), January 2012.
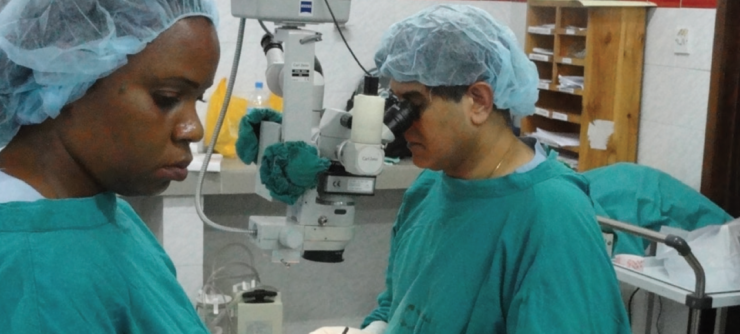
Figure 2. The author operating at CCBRT.
I recall seeing a patient during my most recent visit, when unfortunately I did not have time to operate. He had already had a lamellar transplant for extremely advanced keratoconus in one eye (Figure 3) and was waiting for the other eye to be treated. I spoke to him in Swahili and apologized that I was not able to operate on his other eye at that visit, but he answered that he was grateful and thankful to have had his first eye treated, as it gave him his life back. Because of that surgery, he was able to go back to his job as a schoolteacher and had a restored sense of confidence. He had lost his job because of poor eyesight and had had no income for more than 8 years. This is only one of many encounters that remind me how privileged we are to be in a position to transform the lives of others.
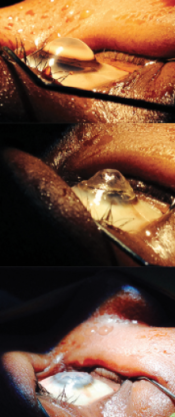
Figure 3. Deep anterior lamellar keratoplasty on an eye with extreme keratoconus.
In 2003, while I was treating patients at CCBRT, one developed a case of endophthalmitis. I was surprised at how relaxed everyone was, and I was then alarmed to learn that this was a regular occurrence, with clusters of endophthalmitis occurring almost every month. I introduced them to intracameral cefuroxime, and they subsequently did not see a single case in 3 consecutive years, across 21,000 procedures.4
My frustration, however, has been the low overall impact in terms of numbers that one can achieve. At the most, I have been able to perform corneal transplantation in 15 patients at one time. This is a difficult problem to solve because of the poor availability of corneal tissue. Training local ophthalmologists in advanced corneal techniques would make a sustainable difference, as long as they were able to keep up their skills and train others—not really viable without easy access to corneal tissue.
One of my most memorable trips was to Burma, in 1994, where I accompanied my Burmese colleague Wilbert Hoe, FRCOphth, and nurse Hillary Welling (Figure 4). We did the first phacoemulsification in the country in a room that had been converted into an operating theater within a Buddhist monastery in the Sagaing Hills. It was a magical time, living in the monastery, operating on monks and nuns, and spending time visiting the country. We performed a large number of cataract surgeries—more than 150—with support from local medical ophthalmologists and personnel. That location has since become a center for eye care, with numerous international ophthalmologists visiting. Since that time, the Abbot of the monastery, Venerable Ashin Nyanissara, has established more than 30 eye centers throughout Burma. Four years ago, I had the honor of performing bilateral simultaneous cataract surgery on the Abbot in my practice. I implanted trifocal lenses in both of his eyes (Figure 5).
Figure 4. Nurse Hillary Welling, assisting the author in performing the first phacoemulsification in Burma, 1994.

Figure 5. The author and the Abbot of the monastery, Venerable Ashin Nyanissara.
THE JOURNEY CONTINUES
The anecdotes told in CRST Europe this month are heartfelt, but they tell only part of our journey in restoring sight—a journey that is emotional for us all. There is much yet to accomplish when it comes to world blindness. It is wonderful to see the contributions made by so many colleagues who, in their own way, and with their own skills—whether leadership, organizational ability, project management, fund-raising, education, or just direct hands-on effort—work with compassion to reduce blindness.
Congratulations to everyone who has undertaken efforts in the fight against world blindness, and long may these efforts continue. Safari Njema, which means “safe travels” in Swahili.
1. World Health Organization website. Visual impairment and blindness fact sheet. http://www.who.int/mediacentre/factsheets/fs282/en/. Accessed April 3, 2017.
2. Sight Aid International website. http://www.sightaidinternational.org/. Accessed April 3, 2017.
3. Resnikoff S, Felch W, Gauthier TM, Spivey B. The number of ophthalmologists in practice and training worldwide: a growing gap despite more than 200,000 practitioners. Br J Ophthalmol. 2012;96(6):783–787.
4. Wood M, Bowman R, Daya SM. Prophylactic cefuroxime and endophthalmitis in Tanzania, East Africa. J Cataract Refract Surg. 2008;34(1):9-10.
Sheraz M. Daya, MD, FACP, FACS, FRCS(Ed), FRCOphth, Chief Medical Editor



