
We were in a small, very poor village in Sierra Leone. This was in the 1980s, and I was there taking part in a trial of ivermectin for onchocerciasis, or river blindness. As we traveled around dispensing the medication and assessing its effectiveness, I had my first exposure to seeing blind people in Sub-Saharan Africa in their communities and in their homes. In this particular village, I noticed that a group of blind adults was sitting under a tree when we came into the village, and they were still sitting under the same tree when we left the village, doing absolutely nothing.
In another village, we approached a group of women who were engaged in an activity. My attention was drawn to a child who was rocking back and forth, back and forth. As I got closer, I realized that she was blind from corneal scaring. She was rocking because she was so understimulated. I learned that she had been blinded by measles when she was 5 years old, and she was now a teenager. For 8 years, she had been in that village doing nothing: no schooling, no activity, no friends, just sitting with the adults or rocking back and forth, doing nothing.
These observations had a profound impact on me. At that point, I had been a clinical ophthalmologist in the United Kingdom for 10 years, and I had seen people in a sanitized hospital environment where the main focus is on the eyes. I knew nothing, or next to nothing, about my patients’ context or the impact of their visual limitations on their relationships, their work, or their interests. Seeing those blind people, idle in their home villages, provided me with a lifetime of motivation to look for ways to prevent blindness, especially in children. I have spent the rest of my career to date in that pursuit (Figures 1–7).

Figure 1. Children at a school for the blind in Thailand, many of whom were blind from ROP.

Figure 2. These children, found in a slum in Chittagong, Bangladesh, underwent successful cataract surgery thanks to a large program that came about as a result of the PhD work of an ICEH alumnus.

Figure 3. Regional workshop in ROP for Latin America, which took place in Panama.
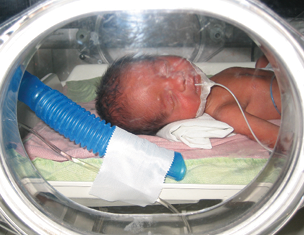
Figure 4. Preterm infant in an incubator in Venezuela, being given 100% oxygen through the blue tube.
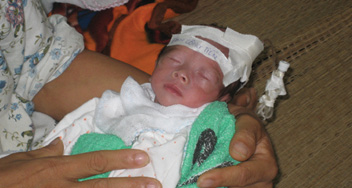
Figure 5. Preterm infant in Vietnam who had just been treated for ROP.

Figure 6. Neonatal nurses discussing the challenges they face in caring for preterm infants as part of a study to assess the impact of training nurses on rates of ROP in Rio de Janeiro, Brazil.

Figure 7. 2013 National ROP Summit, Delhi, at which strategies for the Queen Elizabeth Diamond Jubilee Trust were agreed upon.
DUTIES VARIED BUT RELATED
I joined the International Centre for Eye Health (ICEH), which is now located at the London School of Hygiene and Tropical Medicine (LSHTM), in 1990, where I am a Professor of International Eye Health. My duties fall into three broad areas: research and dissemination of the findings, education, and providing technical advice to nongovernmental organizations (NGOs) on blindness prevention efforts.
Research. I lead a group conducting research into blinding eye diseases, focusing on low- and medium-income countries. My particular research interest is blinding eye diseases in children. I have also been involved in four national surveys of blindness in adults, and I am now focusing on research into glaucoma in adults in Africa—a neglected topic.

Education. I teach in the Masters course at the ICEH, one unit on blinding eye diseases in children and another on skills for field research in eye care. Additionally, I contribute to courses at the LSHTM on tropical eye disease and other topics. I also contribute articles to the Community Eye Health Journal, a quarterly publication with a circulation of 30,000 that is translated into five languages. The ICEH also supports a program called Links, which puts eye care departments in the United Kingdom in partnership with eye care departments in developing countries, principally in Africa but also elsewhere, to improve the quality and quantity of eye care training.

Technical advice. The greatest share of my time in this area is spent giving advice to the Queen Elizabeth Diamond Jubilee Trust , which is supporting efforts to eliminate avoidable blindness throughout the countries of the Commonwealth. I am advising them on national programs for control of diabetic retinopathy and retinopathy of prematurity (ROP) in India. I also provide input to the USAID Child Blindness Program and others.
These duties may seem varied, but they all relate one to another. For example, I often work with and learn from our alumni after they graduate. I am currently working with one alumnus who just finished his PhD and two other alumni for whom I was PhD supervisor for degrees awarded this past year. The results of research can often be fed straight into the Masters course I teach, so that current students can benefit from the latest research findings. Further, we often ask our alumni to write articles for the Community Eye Health Journal summarizing the findings of relevant research or programs they are involved in, which are then disseminated in several languages, broadening the reach of what our students or alumni have learned. My work as a technical advisor to different organizations also provides other occasions for sharing the findings of our research, to inform policy or program planning. So these elements overlap and complement each other to make a very nice whole.
THE PATH TO A CAREER
I am a very visual person—a frustrated artist—so vision to me is incredibly important. That is one of the reasons I chose ophthalmology as a career. As for going into international health, I can thank my parents for that. My mother was a nurse in the army during World War II, and she worked in East Africa and India. My father, who worked in personnel, spent time in Tanzania after World War II. When I was a child, hearing stories about what they did and why they did it really whetted my appetite for working overseas.
Initially I thought I wanted to be an ophthalmologist working somewhere in Africa. I quickly realized, however, that, although that work is important and for many people those interventions are life-changing events, that was not what I wanted to do. A key turning point came when I was training in the United Kingdom as a vitreoretinal surgeon. A colleague whom I had known for a long time and who had worked in Africa was recruiting ophthalmologists for one of the early trials of ivermectin for river blindness in Sierra Leone. That led to the incident I related at the beginning of this article.
I joined that team and spent 6 months in Sierra Leone, walking long distances, carrying equipment, and trying to do rigorous research in the very poor, dysfunctional country, as it was at that time. That experience allowed me to see how research could help provide answers to questions that could then revolutionize care, particularly in the realm of public health. The evidence provided by those early trials—one in Cameroon, the one I was involved in Sierra Leone, and one in Nigeria—led to the development of the African Programme for Onchocerciasis Control, one of the most successful programs in history, resulting in the prevention of an estimated 40,000 cases of blindness every year.1
That experience was what led me into a career in international ophthalmology and public health. I was fortunate after my experience in Sierra Leone that a position became available at the ICEH, and I just walked right into it in 1990. The remit I was given was to investigate the causes of blindness in children. There was increasing evidence on the major causes of blindness in adults, but there was little evidence on blinding eye diseases in children. That has since been the main theme in my research and interests.
EFFORTS IN ROP
In the late 1990s, as we collected data by examining blind children from all over the world, it became apparent that ROP was a major cause of blindness in children in Latin America. In 1997, we held the first workshop for ophthalmologists across the region on ROP. At that time, we were able to identify only two ophthalmologists in the region who were screening for or treating ROP. Subsequently, Chile was the first country to develop a national program for ROP, based on data that we had collected in Latin American countries, including Chile.
Since 1997, I have been to Latin America 15 times for national or regional ROP workshops. Over the years, thanks to local support from the German NGO Christoffel Blindenmission in particular and wonderful leadership within Latin America, every country in Latin America now has a program for ROP. Levels of quality and coverage vary, but several countries now have national guidelines and several have legislation mandating that all premature babies should be examined for ROP.
At a certain point, the challenges these countries faced were no longer technical but more political and financial, which I cannot really influence. When that became apparent, I shifted my attention to Eastern Europe. With support from the International Agency for the Prevention of Blindness, I have been to Russia several times and have helped facilitiate a regional workshop in Georgia and workshops in other countries in Eastern Europe.
Experiences and learning from these other countries is feeding into the work on ROP in India that is being supported by the Trust, as mentioned previously. My hope is that, based on experiences in Latin America and Eastern Europe, efforts will be scaled quite quickly, given the great expertise and leadership that exists in India.
FORTUNE FAVORS THE BRAVE
All things considered, I have been fortunate to be the right person, in the right place, at the right time, with a great deal of support from the fantastic colleagues that I have met and worked with. We work well as a team, and this is vital no matter where you are working. The best research ideas come to us as a result of discussion, and determining how the research will take shape is best formulated through further discussion. Having a supportive team is key to all this.
Personally, it has been extremely rewarding to work with a wide range of people of different religions and from different cultures and to see health systems in other parts of the world. It is fascinating, and I am constantly learning. It is a great privilege to support researchers, whether ICEH students or PhD students, to see them flourish and to go on to positions of leadership and become independent researchers.
It also must be said that I have the most amazingly supportive husband, without whom my work in international ophthalmology would not have been possible.
Often junior doctors come to me and say they would like to go into international ophthalmology, but it means making a tough decision between having a career at home or doing something quite different and less secure. I tell them, “Fortune favors the brave.” If this is what you really want to do with your life, then do it. If your head and your heart are aligned, this is where your energy lies, and you can be open to opportunity. I think this is worthwhile advice for anyone to heed.
1. Prevention of Blindness and Visual Impairment: African Programme for Onchocerciasis Control (APOC). World Health Organization. http://www.who.int/blindness/partnerships/APOC/en/. Accessed April 4, 2017.



