

Blindness and significant visual impairment from cataracts affect approximately 100 million people worldwide. Compassionate and ethical medical care can have a positive impact on the blind poor and their families, community, and country. Approximately 90% of these disadvantaged individuals live in developing countries, where they face both geographic and economic barriers to receiving cataract surgery.
When teaching students (university, medical, and nursing), residents, fellows, and board-certified ophthalmologists, we discuss the virtue of service. We explain that there are those who consume and those who contribute, those who look down on others and those who lift others up. Ethical global humanitarian ophthalmology projects raise up the disadvantaged. Restoring sight may allow a poor individual to lead a self-sustainable life.

Figure 1. At 4 years old, Litia was blind from cataracts (Figure at outset). On the morning after bilateral cataract surgery, her eyes were wide open and looking straight ahead (above).
Ophthalmologists who wish to address the global problem of curable blindness must follow a code of ethics. They also must strive to deliver care that is in the best interest of each patient, no matter where the service is provided.
ETHICAL GUIDELINES FOR HUMANITARIAN OPHTHALMOLOGY
No. 1: Competence. During ophthalmology training, attending physicians oversee the work of residents and take over if necessary to ensure a good result. We work in a similar fashion in the mission field.
No. 2: Informed consent. Through a translator, we explain to patients that it is their choice to undergo surgery as part of the informed consent process.
No. 3: Approved products only. There is no testing of unapproved products on patients during our humanitarian projects.
No. 4: Preoperative examination. Patients are assessed before treatment or surgery, and management decisions are made based on their best interest with no pressure or time constraints.
No. 5: Guidance. Residents who prescreen patients discuss the disposition of care but do not proceed without the approval of the attending physician.
No. 6: Postoperative care. Patients receive postoperative instructions in writing and verbally, usually when a family member is present. Patients are instructed to return to the clinic for follow-up appointments. Local hosts for these projects receive patients’ contact information. Those with postoperative concerns receive follow-up medical care and guidance via telemedicine through the host conduit.
No. 7: Professional arrangement. Humanitarian projects are established and confirmed with in-country local government, physicians, and leaders.

Figure 2. Eleven-year-old Elizabeth was born blind (A). Her mother’s deepest wish was that Elizabeth be able to see the world and to run without falling and cutting and bruising her legs. Giving her the gift of sight was an awesome privilege (B).

Figure 3. Tasi was the only teacher at his village’s school. Blind from cataracts, he lost his life’s purpose (A). After cataract surgery, he said his life was worth living again, and he resumed teaching children in Samoa (B, C).
We adhere to these guidelines, but there are physicians who set up humanitarian projects without incorporating ethical guidelines. In our experience, this approach is fraught with potential problems, including lack of patient consent and the creation of a project not approved by local physicians and governmental authorities. The volunteering physicians may also lack experience with medical mission equipment such as portable operating microscopes and techniques such as manual small-incision cataract surgery (MSICS). Lack of knowledge and/or insufficient research and planning for humanitarian international eye surgical mission projects can lead to surgical complications, ill will, and a distrust of future humanitarian ophthalmologists.

Figure 4. Bilateral blinding cataracts (A) prevented husband and wife Ramesh and Onaradah from seeing each other for 8 years (B).
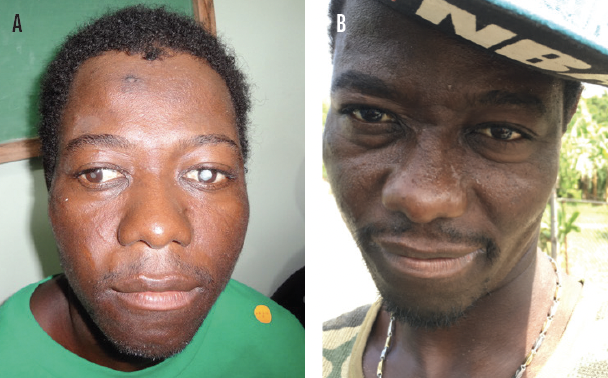
Figure 5. Emilio was 30 years old at presentation. He had been born blind, which had led to significant exotropia. Emilio had been raised by nuns, who said he had no interest in anything. During the preoperative examination, he did not respond to any questions posed through a translator, and his mental capacity appeared to be limited (A). Surgery provided him with good vision and eliminated the exotropia. Emilio was able to leave behind a life of begging and obtain his first job (B).
LESSONS LEARNED IN THE FIELD
No. 1: Bring your own instruments. The instruments available on humanitarian projects often do not include all those you are used to, which can create a surgical dilemma in the middle of a case.
No. 2: Be competent at performing MSICS or work with someone who is. On humanitarian trips, 4+ dense nuclear sclerotic cataracts are the norm. We label these unphaco-able.
No. 3: Brush up on suturing techniques. Many cataract surgeons, especially residents and fellows, have not had to place sutures during cataract or pterygium surgery in a long time.
No. 4: Download some videos. It can be useful to have on your smartphone, tablet, or laptop videos of any procedure you may be performing, such as MSICS, severe ectropion/entropion surgery, and strabismus surgery.
No. 5: Do not perform a procedure you do not feel confident performing. It is better not to operate than to operate and leave a patient with a severe complication such as a dropped nucleus, retinal detachment, endophthalmitis, or ocular sutures that must be removed weeks after you have left. Therefore, avoid attempting to perform a procedure you do not routinely perform in your practice unless you are being guided by an expert who is willing to closely oversee your work in the OR and take over at a moment’s notice.
No. 6: Do not perform a procedure that requires follow-up that you or a competent ophthalmologist will not be able to provide. The surgical outcome will not be successful, and the patient will be worse off.
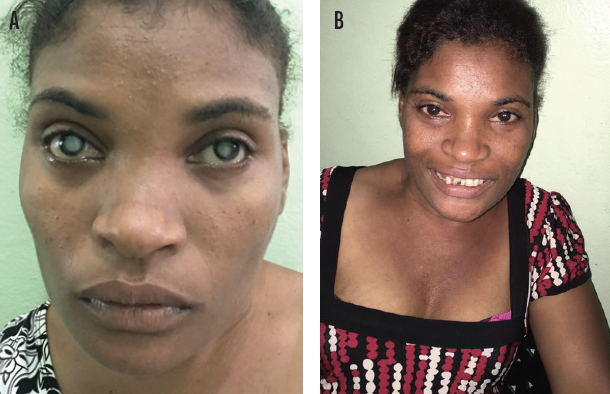
Figure 6. While pregnant with her, Trinidad’s mother developed a viral infection. This left Trinidad with profoundly dense white cataracts and possible retinal scars (A). Six months after surgery, she traveled 5 hours by bus to thank one of the authors (J.J.R.). She had gotten her first job and was a caregiver for small children (B).
A WORTHWHILE EXPERIENCE
Participating in global ophthalmology can be one of the most worthwhile and rewarding opportunities in an ophthalmologist’s career. It can also be a humbling experience.
We return annually to several communities in developing countries. To our minds, this is the best way to proceed in global humanitarian ophthalmology. It has allowed us to build long-lasting bonds with our humanitarian eye team and these communities (Figures 1–6). This, in turn, has created wonderful opportunities for us to help people move out of the depths of poverty.



