Hyperopic LASIK Remains a Viable Treatment Option
This procedure is especially valuable for young patients and early presbyopes.
By Diego de Ortueta, MD, FEBO
Some readers of this article may question whether hyperopic LASIK remains a viable refractive surgery option. On one hand, the treatment is limited because of its creation of optical aberrations, including spherical aberration and coma. On the other hand, I would argue, hyperopic LASIK continues to serve some patient populations that are not well-suited to other refractive surgical approaches.
Regarding the effect of induced aberrations, it is known that negative spherical aberration can provide patients with greater depth of focus. This is well-suited to the hyperopic population because it allows patients to read better without glasses. In fact, this principle is incorporated into some laser ablation platforms. For example, on the Amaris excimer laser platform (Schwind eye-tech-solutions) that I use, the surgeon can vary the amount of spherical aberration in each eye by manipulating the amount of near addition programmed into the PresbyMax software.
Other aberrations induced by hyperopic treatments, such as coma, may result in diminution of visual acuity, and therefore treatments should be planned so as to minimize these. Although neural adaptation can mitigate some of the effects of aberrations, changes in higher-order aberrations (HOAs) may result in diminution of patients’ visual quality.1
IMPROVED PROFILES
In myopic ablation profiles, the central cornea is flattened relative to the periphery. Hyperopic profiles are more complex, however, because the center must be made steeper relative to the periphery. This has presented a challenge in relation to the design of hyperopic ablation profiles.
Improved ablation profiles (aberration neutral, aspheric, and wavefront-optimized) have been designed to account for the loss of energy due to reflection losses (Fresnel equations) dependent on the laser’s angle of incidence and for loss of efficiency dependent on geometric distortion (ie, angle of incidence).2 Peripheral ablation in hyperopic LASIK is subject to a loss of energy. One method to address this loss is to determine preoperative keratometry (K) readings at several meridians and adjust the ablation algorithm and the number of laser spots based on the geometry of the cornea. With this method, a steeper cornea would require more pulses than a flatter cornea, as the spot geometry changes with the incident curvature.
We compared the induction of corneal aberrations after hyperopic LASIK up to 6.00 D with an aspheric-optimized or aberration-neutral (aberration-free) profile versus conventional ablation. The main differences between the two profiles were that the aberration-free profile incorporated the preoperative K values and calculated the loss of the energy at the periphery. We found that eyes treated with the aberration-free profile had lower induction of HOAs compared with eyes treated with conventional ablation.3
CENTRATION OF HYPEROPIC ABLATION
The shape of hyperopic ablations is more sensitive to subtle decentration than myopic ablation profiles. The effect of decentration may be more pronounced in hyperopic eyes due to the larger angle kappa in these eyes.
THREE APPROACHES TO CENTRATION:
.
Controversy exists regarding the best approach to centration of hyperopic ablations (see Three Approaches to Centration). Most eye-tracker systems use the center of the pupil as a reference. However, the pupil center changes with the diameter of the pupil (centroid shift). By contrast, the corneal vertex is a morphologic landmark that remains stationary during treatment and is reliable and reproducible with corneal topography. In one study, we found that standard hyperopic LASIK could achieve good predictable efficacy and safety when the ablation center was shifted to the cornea vertex.4
Reinstein and colleagues performed a study centering hyperopic LASIK on the coaxially sighted corneal light reflex using a standard nonwavefront-guided ablation profile. Their results provided evidence that refractive corneal ablation should not be systematically aligned with the entrance pupil center.5
OTHER ISSUES
Another factor that has been related to the impact of spherical aberration on LASIK outcomes is the surface smoothing that takes place as a result of corneal wound healing.6 The thickness of the epithelium can change in the cornea’s effort to reestablish a smooth optical surface, and this may partially mask the presence of an irregular stromal surface.
Stability has also been a concern in hyperopic LASIK. Stability can be defined from the manifest refraction, but it would be better to have an objective measurement. We have used changes in corneal topography as objective data to measure the refractive power change in hyperopic LASIK.7 This allowed us to differentiate regression from latent hyperopia, which becomes manifest over time after the treatment. In this study, we observed regression between months 3 and 36 only at the 7-mm zone for an optical zone of 6.5 mm, and this was not correlated with the intended refraction. No significant regression was seen at 3- or 5-mm K readings.
LASIK Xtra IN HYPEROPIA
Several studies in highly myopic eyes have demonstrated that LASIK combined with CXL, a procedure known as LASIK Xtra, can provide refractive and keratometric stability.8,9 Although increased keratometric stability would be desirable in hyperopic LASIK, in my opinion there is reason to have reservations about using the LASIK Xtra technique in hyperopic patients. (Editor’s Note: In the accompanying article on the following page, LASIK Xtra is described in more detail.)
One of the known effects of CXL is the flattening of the cornea over time.10 In hyperopic LASIK, the goal of the procedure is corneal steepening. If CXL causes corneal flattening, this would lead to production of hyperopia, negating some of the effect of the LASIK treatment. Another element that warrants study is what effect CXL has on the growth of the corneal epithelium after hyperopic LASIK. Further caution is advisable regarding the possible effects of CXL on the corneal flap in LASIK, such as shrinkage or folds.
CONCLUSION
Hyperopic LASIK will survive mainly for treatment of the young population. For those who need glasses for refractions of 3.00 to 6.00 D and for those around age 40 years, when small amounts of hyperopia begin to cause problems for far vision, hyperopic LASIK can be valuable. In the latter group, we can also add a small amount of negative spherical aberration with PresbyMax software, so that the need for reading glasses can be delayed or dependence on them reduced.
1. Azar DT, Primack JD. Theoretical analysis of ablation depths and profiles in laser in situ keratomileusis for compound hyperopic and mixed astigmatism. J Cataract Refract Surg. 2000;26:1123-1136.
2. Arba-Mosquera S, de Ortueta D. Geometrical analysis of the loss of ablation efficiency at non-normal incidence. Opt Express. 2008;16(6):3877-3895.
3. de Ortueta D, Arba Mosquera S, Baatz H. Aberration-neutral ablation pattern in hyperopic LASIK with the ESIRIS laser platform. J Refract Surg. 2009;25:175-184.
4. de Ortueta D, Schreyger F. Centration on the cornea vertex normal during hyperopic refractive photoablation using videokeratoscopy. J Refract Surg. 2007;23(2):198-200.
5. Reinstein D, Gobbe M, Archer TJ. Coaxially sighted corneal light reflex versus entrance pupil center centration of moderate to high hyperopic corneal ablations in eyes with small and large angle kappa. J Refract Surg. 2013;29(8):518-525.
6. Reinstein DZ, Archer T. Combined Artemis very high-frequency digital ultrasound-assisted transepithelial phototherapeutic keratectomy and wavefront-guided treatment following multiple corneal refractive procedures. J Cataract Refract Surg. 2006;32:1870-1876.
7. De Ortueta D, Arba-Mosquera S. Topographic stability after hyperopic LASIK. J Refract Surg. 2010;26(8):547-554.
8. Kanellopoulos AJ, Asimellis G, Karabatsas C. Comparison of prophylactic higher fluence corneal cross-linking to control, in myopic LASIK, one year results. Clin Ophthalmol. 2014;8:2373-2381.
9. Tan J, Lytle GE, Marshall J. Consecutive laser in situ keratomileusis and accelerated corneal crosslinking in highly myopic patients: preliminary results [published online ahead of print December 5, 2014]. Eur J Ophthalmol.
10. Kanellopoulos AJ, Asimellis G. Keratoconus management: long-term stability of topography-guided normalization combined with high-fluence CXL stabilization (the Athens Protocol). J Refract Surg. 2014;30(2):88-93.
Diego de Ortueta, MD, FEBO
- Senior Consultant, Aurelios Augenzentrum, Recklinghausen, Germany
- diego.de.ortueta@augenzentrum.org
- Financial disclosure: Consultant (Schwind eye-tech-solutions)
LASIK Xtra: A New Option for Hyperopia Correction
Combination of laser ablation and CXL strengthens the treatment.
By Pavel Stodulka, MD, PhD
LASIK is a widely practiced and well-accepted refractive surgical solution with benefits that have been enjoyed by millions of patients around the world. However, most of the beneficiaries of LASIK have been myopes and astigmatic myopes. Use of LASIK for correction of hyperopia and hyperopic astigmatism has lagged behind these other applications. For example, a review of outcomes of excimer laser refractive surgery included greater than 10 times more eyes corrected for myopia (785 eyes; 91.8%) than for hyperopia (70 eyes; 8.2%).1
One of the possible reasons for the lower rate of acceptance of hyperopic LASIK may be higher rates of regression and retreatment compared with myopic correction. In that same review, the authors reported that hyperopic eyes were significantly more likely to undergo retreatment (P=.006).
The challenge of creating hyperopic treatments on the cornea is that the cornea must be steepened centrally, as opposed to flattening in myopic treatments. This can lead to loss of effect of the surgery over time because of the impaired corneal biomechanical stability and the epithelial masking effect.
combination treatment
The use of CXL in combination with LASIK, dubbed LASIK Xtra, has been proposed as a way to enhance corneal biomechanical integrity and stabilize the cornea after LASIK, as well as to lower the risk of iatrogenic ectasia. LASIK Xtra, according to our Prague protocol, not only increases the stability of the residual corneal stroma but also makes the flap stiffer. This should contribute to a more even-shaped anterior corneal surface, as it is formed by the flap and folded over the steep hyperopic profile ablated by the excimer laser. If LASIK Xtra is shown to improve the dependability of results in hyperopia correction, this may lead to a new level of acceptance of the technique by patients and surgeons alike.
Comparing LASIK Xtra Protocols
Standard Protocol
In the standard protocol for LASIK Xtra, after refractive correction has been performed using the surgeon’s usual approach to hyperopic LASIK but before the flap is replaced, a riboflavin formulation (Vibex Xtra; Avedro) is applied to the exposed corneal stromal bed for 1 minute. The riboflavin is rinsed from the cornea with balanced saline solution. The LASIK flap is then replaced, and UV-A light from the KXL system (Avedro) is applied through the intact epithelium. Exposure time is 75 seconds at a power of 30 mW/cm2.
Prague Protocol
In the Prague protocol for LASIK Xtra, riboflavin is applied to the stromal bed, but it is not rinsed with balanced saline solution. The flap is repositioned, and then more riboflavin is injected under the flap. After a waiting time of 10 minutes, UV-A light is applied for 90 seconds at 30 mW.
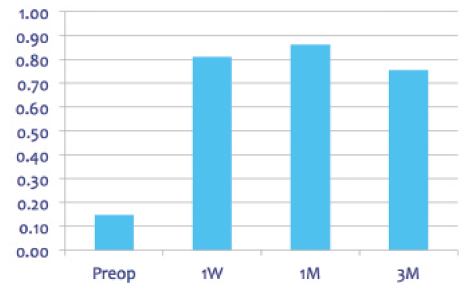
Figure 1. Distance UCVA.
CLINICAL RESULTS
I analyzed the results of 10 hyperopic eyes treated with LASIK Xtra using the Prague protocol. The Prague protocol differs from the standard protocol (both described in Comparing LASIK Xtra Protocols). Mean patient age was 32 years, mean keratometry was 42.78 D, and mean refraction was 3.75 ±0.40 D (range, 1.75–5.25 D). In these procedures, a 140-µm LASIK flap was created with the Victus femtosecond laser (Bausch + Lomb Technolas), and ablation was carried out with the Amaris 750 (Schwind eye-tech-solutions) excimer laser. The CXL portion of the procedure was performed per the Prague protocol described above. Patients completed follow-up visits at 1 week and 1 and 3 months.
At a Glance
- Hyperopic LASIK treatment is limited because of its creation of optical aberrations, including spherical aberration and coma; however, it serves some patient populations that are not well suited to other refractive surgical approaches.
- In one study, standard hyperopic LASIK could achieve good predictable efficacy and safety when the ablation center was shifted to the cornea vertex.
- Hyperopic LASIK will survive mainly for treatment of the young population.
- LASIK Xtra has been proposed as a way to enhance corneal biomechanical integrity and stabilize the cornea after LASIK, as well as to lower the risk of iatrogenic ectasia.
- Potential advantages of the Prague protocol include greater riboflavin penetration, possibly leading to crosslinking in both the stromal bed and flap, and better stability associated with the steep ablation profile.
At final follow-up at month 3, mean refraction was 0.12 ±0.20 D (range, -0.75 to 0.50 D). This was a substantial reduction of hyperopia from the preoperative mean of 3.75 D.
Distance UCVA was good and relatively stable postoperatively, with a mean of better than 0.8 (Snellen decimal) at 1 week and 0.75 at final follow-up (Figure 1). Postoperative distance BCVA was also good and stable, with a mean of approximately 0.9 at 1 week and a similar figure at 3 months.
Safety results were good in these 10 eyes. Two gained 1 line of distance BCVA, five were unchanged from preoperative, three lost 1 line, and no eye lost 2 or more lines.
DISCUSSION AND CONCLUSIONS
Early experience with LASIK Xtra for hyperopia has been promising, according to presentations by multiple investigators at ophthalmic meetings. My initial experience indicates that the Prague protocol has the potential to further increase the advantages of LASIK Xtra in this patient population.
Potential advantages of the Prague protocol include greater riboflavin penetration, possibly leading to crosslinking in both the stromal bed and flap. Additionally, the thick 140-µm flap may lead to better stability associated with the steep ablation profile used in hyperopic laser corrections.
The advantages conveyed by LASIK Xtra may allow the indications for hyperopic LASIK to be expanded. For example, treatment of thinner corneas (minimum, 480 µm) or steeper corneas (up to 47.00 D) may be considered. However, treatment of corneas that are both thinner and steeper would not be recommended at this time. Additionally, the strengthening of the corneal biomechanics imbued by CXL may help to lower the risk of corneal ectasia and stabilize the refractive outcome in hyperopic LASIK. It remains a subject of debate whether CXL should be used universally in conjunction with LASIK as a hedge against iatrogenic ectasia.
CONCLUSION
Early results suggest that LASIK Xtra can be a beneficial procedure for patients with hyperopia who fit inclusion criteria. Longer follow-up and comparison with published data will be needed before this procedure achieves wider acceptance. n
1. Randleman JB, White AJ Jr, Lynn MJ, Hu MH, Stulting RD. Incidence, outcomes, and risk factors for retreatment after wavefront-optimized ablations with PRK and LASIK. J Refract Surg. 2009;25(3):273-276.
Pavel Stodulka, MD, PhD
- Chief Eye Surgeon, CEO of Gemini Eye Clinics, Czech Republic
- stodulka@lasik.cz
- Financial disclosure: Consultant (Bausch + Lomb Technolas)
