The introduction of femtosecond laser technology to cataract surgery has opened numerous avenues for the development of new surgical techniques. By automating the creation of corneal incisions, astigmatic keratotomy incisions, and capsulotomies, and by performing nuclear lens fragmentation and softening, the femtosecond laser allows greater precision and reproducibility.1 The laser’s unique ability to prechop and soften the lens in vivo has enabled us to develop a phaco-free, all-laser technique.2
It has been nearly 50 years since the introduction of phacoemulsification.3 Although significant technological improvements have been made to the technique since then, phacoemulsification remains a source of cataract surgery complications such as endothelial cell loss, corneal edema, capsular rupture, and vitreous loss. Surgical techniques such as phaco chop can reduce the amount of phaco energy and time needed intraoperatively for conventional cataract surgery; however, phacoemulsification still results in endothelial cell loss ranging between 3% and 23%, with most studies averaging around 6% to 7%.4 Endothelial cell loss is a major concern after cataract surgery because of the potential for postoperative corneal decompensation, particularly in patients with preexisting pathology such as Fuchs dystrophy. This often ultimately results in corneal transplantation.5
The rate of capsular rupture for trained cataract surgeons ranges from 1.9% to 5.2% of procedures, with vitreous loss occurring in 1.1% to 5%.6 The rates among ophthalmology residents have been reported to be as high as 16%; however, there is a strong correlation between increased surgical experience and a lower rate of capture rupture, with lower rates among fellows and trained surgeons.7 Capsular rupture and vitreous loss increase the risk of retinal detachment and are associated with worse long-term outcomes. Although capsular rupture can occur at any stage during surgery, phacoemulsification is often the culprit.6
Modern cataract surgery is extremely successful and associated with a low rate of complications. However, if a technique could be developed to eliminate or significantly reduce the use of phacoemulsification, it would represent a significant improvement in the procedure. This article describes one such technique, a phaco-free cataract surgery approach performed with a small incision and use of the femtosecond laser.

Figure 1. The phaco tip is used in I/A mode for aspiration only. No phaco energy is used.
THE PHACO-FREE TECHNIQUE
We have developed a four-step procedure that can be used for cataracts of up to grade 3+ density without the use of phaco energy (see Steps in Phaco-Free Cataract Surgery).
The phaco tip is almost always used for aspiration only, without the application of phaco energy (Figure 1). For cataracts denser than grade 3+ to 4+, the procedure can be modified with the addition of a small amount of phaco energy; we have found this is needed in less than 1% of cases.
For this technique to be successful, we have found that the prechopping, using two mechanical devices to break the lens fragments into small pieces, must be as complete as possible. Traditional phaco chop techniques such as vertical chop are mechanically less efficient for lens fragmentation in this manner, and we have found that a 180° opposing action technique, in which two cracking instruments are positioned 180° from each other, is more mechanically efficient for phaco-free surgery.
Steps in Phaco-Free Cataract Surgery
Step No. 1: Laser. Creation of the capsulorrhexis and lens fragmentation (a cylindrical cut and a crosshair lens cut) using the LenSx laser (Alcon).
Step No. 2: Freeing the lens. Hydrodissecting the lens and floating it into the anterior chamber (Figure 1).
Step No. 3: Prechopping. Mechanically cracking the laser-prechopped lens into small fragments using two choppers or spatulas with an opposing action of 180° (Figure 2); an ophthalmic viscosurgical device is used liberally to protect the corneal endothelium during cracking.
Step No. 4: Chopping. Aspirating lens fragments using a phaco tip (set to I/A mode only) with the assistance of a chopper or spatula to guide and push the lens fragments into the phaco tip (Figure 3).
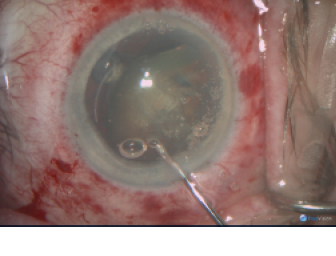
Figure 1. The lens is spun and floated into the anterior chamber in one piece after softening with the femtosecond laser.
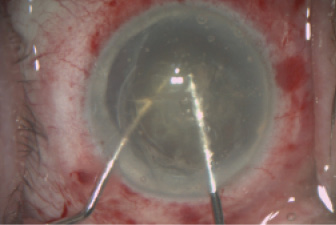
Figure 2. To prepare the lens for aspiration without phaco, the lens is cracked into small pieces mechanically in the anterior chamber using a 180° opposing action.
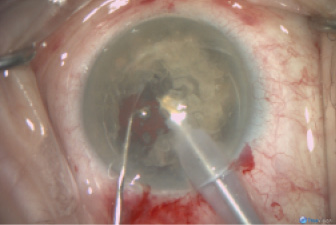
Figure 3. A 1.1-mm diameter phaco tip is used to aspirate the lens fragments without the application of phaco energy. A second instrument is used to guide the fragments.
In the chop step, with the phaco tip in I/A mode assisted by a chopper/spatula, both devices should move toward each other and stay in the center of the anterior chamber as much as possible. For aspiration of fragments, the phaco tip diameter must be as large as possible. The standard phaco tip diameter is 0.9 mm. We use the largest diameter tip commercially available, which is 1.1 mm. For aspiration, we use the highest vacuum level possible (650+ mm Hg).
Before the availability of the femtosecond laser, it was difficult to crack the lens into small enough fragments for aspiration without phaco. With the advent of the femtosecond laser, we have been able to take advantage of the laser’s unique ability to prechop the lens in a closed chamber to soften the lens tissue. This facilitates easy mechanical chopping of the lens for aspiration.
Watch it Now
Ultrasound-Free Laser Cataract Surgery
Using the femtosecond laser to prechop the nucleus enables it to be removed without the use of ultrasound energy.

The femtosecond laser works differently at the deeper tissue level of the lens than it does at the level of the cornea; it is less focused and more diffuse, which results in larger cavitation bubbles. This is undesirable for corneal procedures such as LASIK flap creation, where precision is needed to create a 100-µm flap. However, for lens fragmentation, the large cavitation bubbles increase the area of laser-tissue interaction via a plasma shockwave cavitation bubble mechanism, resulting in a softening of the adjacent lenticular tissue along the cut plane and making this phaco-free technique possible.
In our experience, if too few cutting planes were used in laser lens fragmentation, the lens was difficult to fragment with mechanical cracking. If too many cutting planes were used, the visibility of the capsulotomy edge was reduced. We have found that the optimal femtosecond laser parameters for the phaco-free method are: capsulotomy diameter = 5.25 mm; cylindrical lens cut diameter = 3 mm; and crosshair lens cut diameter = 5 mm. The optimal energy level range for fragmentation is 5 µJ to 15 µJ, depending on lens density. We choose higher levels for denser cataracts to achieve optimal cutting and lens softening. We have found that optimal laser spot separation is between 5 and 9 µm horizontally and vertically.
There are still few peer-reviewed outcome studies regarding results with the femtosecond laser. In a study of 288 patients (225 laser arm, 63 standard arm) who had cataract surgery with the Lensar laser (Lensar) or conventional phacoemulsification, there was a lower rate of endothelial cell loss at 6 months for the laser group (-0.4%) than the conventional group (-2.6%). The study authors theorize that endothelial cell loss was lower due to the reduction or elimination of ultrasonic phaco energy after laser lens fragmentation.6 More research is needed to determine whether complications such as endothelial cell loss or capsular bag rupture will be reduced in a way that is clinically and statistically significant.
AT A GLANCE
- Phacoemulsification remains a source of cataract surgery complications such as endothelial cell loss, corneal edema, capsular rupture, and vitreous loss.
- The femtosecond laser is an effective modality to reduce the amount of phacoemulsification energy used intraoperatively.
- More research is needed to determine whether the reduction of complications such as endothelial cell loss and capsular bag rupture will be clinically or
statistically significant.
CONCLUSION
Using the unique features of the femtosecond laser, we have developed a phaco-free technique for cataract surgery. The femtosecond laser is an effective modality to reduce the amount of phacoemulsification energy needed intraoperatively. We believe that the elimination of phacoemulsification may make small-incision cataract surgery even safer for our patients. n
1. Chang D. Cataract surgery complication rates: how are we doing? Cataract & Refractive Surgery Today. February 2012.
2. Wang M. Phaco-free laser cataract surgery. Cataract & Refractive Surgery Today. March 2012.
3. Kelman CD. Phacoemulsification and aspiration. A new technique of cataract removal. A preliminary report. Am J Ophthalmol. 1967;64(1):23-35.
4. Charters L. Laser cataract surgery incurs less cell loss: endothelial analysis: differences in density more significant with femtosecond laser than conventional phaco. Ophthalmology Times. 2012;37(14):13.
5. Pereira AC, Porfírio F Jr, Freitas LL, Belfort R Jr.. Ultrasound energy and endothelial cell loss with stop-and-chop and nuclear preslice phacoemulsification. J Cataract Refract Surg. 2006;32(10):1661-1666.
6. Lundstrom M, Behndig A, Kugelberg M, Montan P, Stenevi U, Thorburn W. Decreasing rate of capsule complications in cataract surgery: eight-year study of incidence, risk factors, and data validity by the Swedish National Cataract Register. J Cataract Refract Surg. 2011;37(10):1762-1767.
7. Zare M, Javadi M, Einollahi B, Baradaran-Rafii A, Feizi S, Kiavash V. Risk factors for posterior capsule rupture and vitreous loss during phacoemulsification. J Ophthalmic Vis Res. 2009;4(4):208-212.
Nathan Rock, OD
- Consultative Optometrist and Clinical Study Coordinator at Wang Vision 3D Cataract & LASIK Center, Nashville, Tennessee
- DrRock@WangVisionInstitute.com
- Financial disclosure: None
Ming Wang, MD, PhD
- Clinical Associate Professor of Ophthalmology,
University of Tennessee
- Director of Wang Vision 3D Cataract & LASIK Center, Nashville, Tennessee
- International President of Shanghai Aier Eye Hospital, Shanghai, China
- DrWang@WangVisionInstitute.com
- Financial disclosure: None
