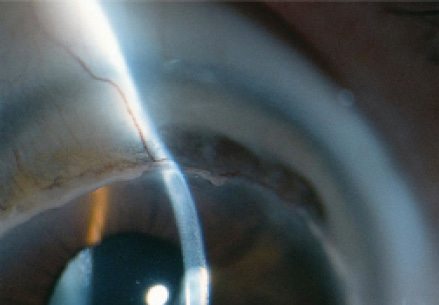
Terrien marginal degeneration (TMD) occurs bilaterally but asymmetrically, with onset usually in middle age or older (see Did You Know? for more characteristics of TMD).1 Diagnosis is made by clinical presentation, which includes progressive peripheral corneal thinning, typically first seen in the superior quadrants, with fine yellowish punctate stromal opacities.
There is no widely accepted approach to treatment of TMD. Lamellar keratoplasty techniques have been proposed but have yet to gain wide acceptance.2,3 Penetrating keratoplasty would not be expected to have a high success rate due to the peripheral nature of the pathology.
CXL has been used safely and effectively to increase corneal rigidity in conditions such as keratoconus and post-LASIK ectasia.4,5 It has also been successful in the treatment of corneal melting.6 In this application, the proposed mechanism of action is an increased resistance to enzymatic digestion in the corneal stroma as a result of CXL.7
With this in mind, Theo Seiler, MD, PhD, and I treated a patient with bilateral TMD using CXL in Zurich, Switzerland, in an attempt to halt and reverse the progression of corneal thinning and melting and to restore the patient's visual acuity.8 This article recaps our successful treatment of that patient.
CASE PRESENTATION
A 47-year-old man was referred to us in 2008 with a diagnosis of TMD. Examination at the slit lamp and Scheimpflug corneal topography provided confirmation of bilateral TMD in the superior corneal periphery.
In the patient's right eye, mean keratometry (K) value in the central 3 mm was 44.40 D, and maximum K (Kmax) was 53.00 D. In his left eye, by contrast, mean K and Kmax values were 50.50 and 81.50 D, respectively. The thinnest corneal points, as determined by Scheimpflug imaging (Pentacam; Oculus Optikgeräte), were 464 µm OD and 414 µm OS. With contact lens correction, distance BCVA was 20/40 OD and 20/63 OS. Following discussion with the patient, it was decided to perform CXL in the worse (left) eye.
Because the pathology was in the superior periphery, the CXL treatment was decentered superiorly, with the area of UV radiation covering the area of melting and thinning. A sponge was used to protect the corneal limbus. The eccentric irradiation was applied according to the Dresden protocol,9 with fluence of 5.4 J/cm2 and settings of 3 mW/cm2 for 30 minutes. Postoperatively, ofloxacin ointment was prescribed every 2 hours during waking hours until reepithelialization was complete, followed by a steroid drop twice daily for 4 weeks.
At a Glance
- A patient with bilateral progressive TMD, treated with CXL using the original Dresden protocol parameters, showed significantly increased K values and marked improvement in distance BCVA in both eyes after CXL.
- The author speculates that the reversal of corneal thinning after CXL in this case caused an increase in resistance to enzymatic digestion in the corneal stroma.
- Although clinical results are limited to two eyes of one patient, with further validation CXL may prove to offer a prophylactic treatment option that can be used when diagnosis of TMD is first confirmed.
DID YOU KNOW?
1. Beauchamp GR. Terrien's marginal corneal degeneration. J Pediatr Ophthalmol Strabismus. 1982;19:97-99.
At 1 year after CXL, mean K and Kmax values OS decreased to 49.00 and 76.60 D, respectively. At 3 years postoperative, these values were 47.70 and 72.70 D, respectively. At 5 years, the mean K remained stable at 47.60 D, but the Kmax decreased to 67.70 D. Distance BCVA was 20/50 at 1 year and 20/32 at 5 years postoperative. By 1 year after CXL, the patient was again able to wear a rigid contact lens in the treated eye. By 5 years postoperative, in 2013, the thinnest corneal point had increased in thickness to 450 µm.
In the meantime, by 2011, the patient's untreated eye showed significant progression, with a mean K of 47.40 D and Kmax of 59.00 D. Distance BCVA with a contact lens was 20/63, and corneal thickness at the thinnest point was 380 µm. Based on the success of the treatment in his left eye, it was decided to perform CXL in his right eye as well.
The second treatment was carried out with the same treatment parameters used in the patient's left eye. By 1 year postoperative, mean K and Kmax values decreased to 46.70 and 56.50 D, respectively, and the thinnest corneal point increased in thickness to 424 µm. By 2 years, these values were 45.70 and 55.40 D, respectively, and distance BCVA was 20/50.
No complications of the treatment have been observed to date in either eye, and the patient is satisfied with his vision and his ability to wear rigid contact lenses in both eyes for about 9 hours a day.
REVERSAL OF THINNING
To the best of our knowledge, this is the first report of TMD being halted clinically, with a follow-up period now of several years. This patient with bilateral progressive TMD, treated with the original CXL Dresden protocol parameters, showed significantly increased K values and marked improvement in distance BCVA in both eyes. More remarkable, perhaps, is the reversal of corneal thinning in the melting peripheral ectatic areas that was seen after the CXL procedures in both eyes. Our speculation is that CXL caused this reversal of corneal thinning.
Our hypothesis for explanation of this phenomenon is that the treatment caused an increase in resistance to enzymatic digestion in the corneal stroma.7 The extracellular matrix in the corneal stroma is held in homeostasis by a balance between collagen synthesis and collagen catalysis. Our assumption is that CXL stopped the catalytic activity, and that, as a result, the balance between synthesis and catalysis of stromal collagen was pushed toward synthesis in the patient's eyes.
CONCLUSION
Although this report includes only two eyes in one patient with TMD treated with CXL, we are encouraged by the promising results. CXL stopped and reversed the progression of corneal melting and thinning in this bilateral TMD patient, who thereby experienced improved visual acuity and renewed ability to wear contact lenses.
Based on these limited clinical results, and subject to further experience and validation, we propose that CXL may be a promising method to avoid keratoplasty and to preserve and restore corneal structure and function in eyes with TMD. It may even offer a prophylactic treatment option that can be used early in the disease course, when diagnosis of TMD is first confirmed. n
1. Beauchamp GR. Terrien's marginal corneal degeneration. J Pediatr Ophthalmol Strabismus. 1982;19:97-99.
2. Bi YL, Bock F, Zhou Q, Cursiefen C. Central corneal epithelium self-healing after ring-shaped glycerin-cryopreserved lamellar keratoplasty in Terrien marginal degeneration. Int J Ophthalmol. 2013;6:251-252.
3. Huang T, Wang Y, Ji J, Gao N, Chen J. Evaluation of different types of lamellar keratoplasty for treatment of peripheral corneal perforation. Graefes Arch Clin Exp Ophthalmol. 2008;246:1123-1131.
4. Raiskup-Wolf F, Hoyer A, Spoerl E, Pillunat LE. Collagen crosslinking with riboflavin and ultraviolet-A light in keratoconus: long-term results. J Cataract Refract Surg. 2008;34:796-801.
5. Richoz O, Mavrakanas N, Pajic B, Hafezi F. Corneal collagen cross-linking for ectasia after LASIK and photorefractive keratectomy: long-term results. Ophthalmology. 2013;120:1354-1359.
6. Schnitzler E, Spörl E, Seiler T. Irradiation of cornea with ultraviolet light and riboflavin administration as a new treatment for erosive corneal processes, preliminary results in four patients [article in German]. Klin Monbl Augenheilkd. 2000;217:190-193.
7. Spoerl E, Wollensak G, Seiler T. Increased resistance of crosslinked cornea against enzymatic digestion. Curr Eye Res. 2004;29:35-40.
8. Hafezi F, Gatzioufas Z, Seiler TG, Seiler T. Corneal collagen cross-linking for Terrien marginal degeneration. J Refract Surg. 2014;30(7):498-500.
9. Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-a-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol. 2003;135(5):620-627.
Farhad Hafezi, MD, PhD
- Chief Medical Officer, The ELZA Institute, Dietikon/Zurich, Switzerland
- Professor of Ophthalmology, Faculty of Medicine, University of Geneva, Switzerland
- Clinical Professor of Ophthalmology, Department of Ophthalmology, University of Southern California, Los Angeles
- info@elza-institute.com
- www.elza-institute.com
- Financial disclosure: None

