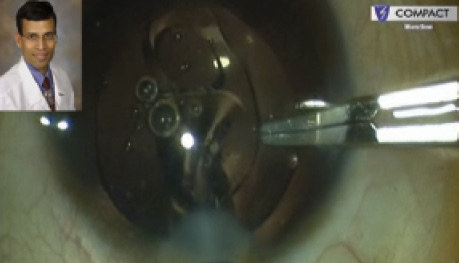
Piggyback IOL implantation, also termedpolypseudophakia, was introduced by Gayton and Sanders in 1993.1 The first report describing the back-to-back placement of two IOLs in a highly hyperopic eye was published by Gills and Fenzl that same year.2
AT A GLANCE
• Primary piggyback IOL implantation provides adequate IOL power in patients with small eyes and/or extreme hyperopia.
• Secondary piggyback IOL implantation is helpful in pseudophakic patients for the correction of residual refractive error.
• Pseudophakic supplementary IOLs are now available for secondary piggyback IOL implantation.
Placing an additional IOL in a piggyback manner is an effective way to correct residual refractive error, particularly when high degrees of refractive surprise are encountered. A review of the literature reveals increasing use of piggyback IOL implantation for the correction of residual refractive errors, along with case reports of complications such as interlenticular opacity and methods to prevent these complications from occurring.1-8 Pseudophakic supplementary IOLs, including Sulcoflex monofocal, toric, and multifocal lenses (Rayner), are now available.
There are two indications for piggyback IOL implantation. Primary polypseudophakia is used in eyes with high hyperopia and short axial lengths that require high IOL powers (eg, nanophthalmos and microphthalmos). Secondary polypseudophakia is used to manage postoperative refractive surprise. This article and accompanying video (www.youtube.com/watch?v=dOBNqOTou7s) overview the fundamentals of piggyback IOL implantation, including the indications, techniques, and complications associated with these procedures.
PREOPERATIVE WORKUP AND PREPARATION
Meticulous preoperative workup and preparation are essential before planning primary or secondary piggyback IOL implantation. The preoperative workup should include thorough anterior and posterior segment examination with an emphasis on IOP, corneal endothelial cell count, and anterior chamber depth. For secondary piggyback IOL implantation, the first IOL should be well centered in the capsular bag. A preoperative Nd:YAG laser peripheral iridectomy or surgical peripheral iridectomy is not needed in most cases; however, it can be performed in patients with shallow anterior chambers or those predisposed to glaucoma.
PIGGYBACK IOL POWER CALCULATIONS
Primary piggyback IOL implantation. Warren E. Hill, MD, has described six steps for IOL power calculation for primary piggyback IOL implantation,9 as detailed below:
- Step No. 1: Measure the axial length accurately;
- Step No. 2: Calculate the total IOL power needed at the plane of the capsular bag;
- Step No. 3: Calculate the residual IOL power;
- Step No. 4: Determine the power adjustment for the
anterior (ciliary sulcus) lens; - Step No. 5: Calculate the power of the anterior IOL; and
- Step No. 6: Select the appropriate lens pair for
polypseudophakia.
Secondary piggyback IOL implantation. For secondary piggyback IOL implantation, IOL power calculations are based on residual refractive error. For myopia, the spherical equivalent is multiplied by 1.15. For hyperopia, the spherical equivalent is multiplied by 1.25.
For more advanced IOL power calculations, we prefer the Holladay Consultant & Surgical Outcomes Assessment software (www.hicsoap.com). This program takes into account residual refractive error, keratometry readings, and anterior chamber depth.
SURGICAL TECHNIQUES
For piggyback IOL implantation, we prefer to implant a three-piece IOL in the ciliary sulcus. Surgeons should never implant square-edged hydrophobic acrylic IOLs in the ciliary sulcus because of the risk of iris chafing and glaucoma. In patients with high hyperopia and short anterior chamber depth, care should be taken to minimize endothelial cell loss by using a chondroitin sulfate–based dispersive OVD, such as DuoVisc or Viscoat (both by Alcon). It is also important to remove all OVD from the anterior chamber after surgery to minimize the risk of postoperative IOP spikes. For additional pearls for managing specific surgical scenarios, see Piggyback IOL Implantation: Case Reports.
CONTRAINDICATIONS
Piggyback IOL implantation should not be attempted in patients with poor endothelial cell count, uveitis, or glaucoma, as this procedure can cause worsening of these preexisting ocular problems.
COMPLICATIONS
Interlenticular opacification, also known as inter-pseudophakosopacification or red rock syndrome, is one complication reported with piggyback IOL implantation. It was first reported in 2000 by Gayton et al,8 who observed the complication in two patients who each underwent implantation of a hydrophobic IOL (AcrySof; Alcon) in the capsular bag through a small capsulorrhexis.
The study authors identified three surgical steps that may help prevent interlenticular opacification: (1) meticulous cortical cleanup, especially in the equatorial region; (2) creation of a relatively large continuous curvilinear capsulorrhexis to sequester retained cells peripheral to the IOL optic within the equatorial fornix; and (3) insertion of the posterior IOL in the capsular bag and the anterior IOL in the ciliary sulcus to isolate retained cells from the interlenticular space.10
PIGGYBACK IOL IMPLANTATION: CASE REPORTs
Case No. 1: Refractive Lens Exchange and Primary Piggyback IOL Implantation for High Hyperopia
Case No. 2: Primary Piggyback IOL Implantation for Developmental Cataract
Case No. 3: Secondary Piggyback IOL Implantation of Supplemental IOL
CONCLUSION
Primary piggyback IOL implantation provides adequate IOL power in patients with small eyes and/or extreme hyperopia. Secondary piggyback IOL implantation is helpful in pseudophakic patients for the correction of residual refractive error. Pseudophakic supplementary IOLs such as the Sulcoflex are now available for secondary piggyback IOL implantation. Combination of monofocal, toric, and/or multifocal IOL implantation in a piggyback manner is a viable and useful option for eyes that require very high IOL powers.
1. Gayton JL, Sanders VN. Implanting two posterior chamber intraocular lenses in a case of microphthalmos. J Cataract Refract Surg. 1993;19:776-777.
2. Gills JP, Fenzl RE. Piggyback IOL implantation.J Cataract Refract Surg. 1993;19:776-777.
3. Rubenstein JB. Piggyback IOLs for residual refractive error after cataract surgery. Cataract & Refractive Surgery Today. August 2012.
4. Holladay JT, Gills JP, Leidlein J, Cherchio M. Achieving emmetropia in extremely short eyes with two piggyback posterior chamber intraocular lenses. Ophthalmology. 1996;103:1118-1123.
5. Shugar JK, Lewis C, Lee A. Implantation of multiple foldable acrylic posterior chamber lenses in the capsular bag for high hyperopia. J Cataract Refract Surg. 1996;22:1368-1372.
6. Shugar JK, Schwartz T. Interpseudophakos Elschnig pearls associated with late hyperopic shift: a complication of piggyback posterior chamber intraocular lens implantation. J Cataract Refract Surg. 1999;25:863-867.
7. Shugar JK, Keeler S. Inter-pseudophakos intraocular lens surface opacification as a late complication of piggyback acrylic posterior chamber intraocular lens implantation. J Cataract Refract Surg. 2000;26:448-455.
8. Gayton JL, Apple DJ, Peng Q, et al. Interlenticular opacification: A clinicopathological correlation of a new complication of piggyback posterior chamber intraocular lenses. J Cataract Refract Surg. 2000;26:330-336.
9. Hill W. Calculating for primary polypseudophakia. http://www.doctor-hill.com/iol-main/polypseudophakia_calculations.htm. Accessed April 18, 2016.
10. Werner L, Shugar JK, Apple DJ, et al. Opacification of piggyback IOLs associated with an amorphous material attached to interlenticular surfaces. J Cataract Refract Surg. 2000;26:1612-1619.
Suresh K. Pandey, MBBS, MS
• Director, SuVi Eye Institute & LASIK Laser Centre, Kota, Rajasthan, India
• Visiting Assistant Professor, John A. Moran Eye Center, University of Utah, Salt Lake City
• Visiting Surgeon, Sydney Eye Hospital, Save Sight Institute,University of Sydney, Australia
• suresh.pandey@gmail.com
• Financial interest: None acknowledged
Vidushi Sharma, MD, FRCS
• Director, SuVi Eye Institute & LASIK Laser Centre, Kota, Rajasthan, India
• suvieye@gmail.com
• Financial interest: None acknowledged