
Capitalizing on technology allows doctors to take our oath to “do no harm” to a higher level. One good technology plus another good technology creates a synergy that we all strive for—safer, more effective surgery with lower downside potential. By marrying technologies, we create a safety zone, increasing our confidence and ability to minimize complications, even in the most difficult cases. This article presents two case studies that illustrate this point.
CASE no. 1
A 67-year-old woman presented with congenital zonular dehiscence, which, under a widely dilated pupil, indicated a visibly scalloped edge along 3 to 4 clock hours. The lens also shifted to the other side and lacked adequate zonular support. The patient’s presurgical BCVA was 20/50.
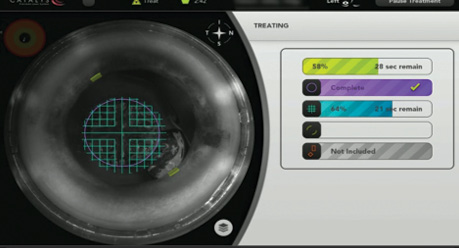
Using the Catalys Precision femtosecond laser (Abbott Medical Optics), centration of the capsulotomy was automatically calculated. When the treatment was done, it appeared off-center; however, once the capsular tension ring (CTR) was inserted, a perfectly centered capsulotomy was apparent. This crucial step was rendered far simpler because the laser system has the ability to calculate placement despite the initial decentration of the patient’s lens. Next, the surgeon used the laser to perform complete segmentation and softening of the nucleus, which substantially reduced manipulation during lens removal and helped prevent damage to any additional zonules. Phacoemulsification using the venturi pump mode on the WhiteStar Signature (Abbott Medical Optics) allowed nuclear fragments to flow easily into the phaco tip.
The ability to flip on the fly from peristaltic to venturi pump mode permitted a safe distance between the phaco probe and the fragile capsule, thus minimizing risk caused by stress or tension on or manipulation of the capsule. The surgeon inserted a CTR to stretch the lens capsule into an ideally shaped, round, centered capsule allowing implantation and a perfectly centered IOL. The patient had a postoperative BCVA of 20/30, and no new zonular damage was caused. The pairing of these technologies produced a great outcome for a case carrying a high risk for capsular rupture or the inability to achieve IOL centration.
CASE no. 2
A 73-year-old man presenting with a dense cataract and count fingers at 1 foot BCVA in his right eye underwent surgery using the femtosecond laser to fragment the nuclei. Laser fragmentation can contribute to the safety of the procedure by reducing or even eliminating the amount of ultrasound energy required to carve, crack, and disassemble the nucleus. A 20-gauge MST/Dewey large-bore phaco tip (30º bend, 0.7-mm diameter, and 0.9-mm outer diameter; MicroSurgical Technology) was used to complement the fluidics of the WhiteStar. By combining the larger-bore tip with the venturi pump mode, the fragments were drawn out and removed without expending any extra phaco energy. The larger internal bore of the phaco needle allowed larger nuclear fragments to be removed without the need for further ultrasound fragmentation. The patient’s postoperative UCVA was 20/25.
In cases involving dense nuclei, emulsification can prove difficult, posing increased risk for eye trauma. These cases carry a much higher risk of pseudophakic bullous keratopathy from endothelial damage and capsular rupture, necessitating some other form of securing the lens, either in the sulcus with a posterior chamber fixated lens or even an anterior chamber IOL. By pairing technologies, the surgeon maximizes the benefits and creates a safer case by preserving the endothelium and zonules, avoiding complications caused by manipulation, and reducing exposure to phaco energy.
At a Glance
• Pairing technologies can create a safer case by preserving the endothelium and zonules, reducing exposure to phaco energy, and increasing the surgeon’s confidence and ability to minimize complications.
• Laser fragmentation can contribute to the safety of the procedure by reducing or even eliminating the amount of ultrasound energy required to carve, crack, and disassemble the nucleus.
• Combining some of the newest innovations can create synergy, allowing a safe and predictable outcome.
Watch it now
John Linn, MD, performs a capsulotomy and phacoemulsification on a patient with congenital zonular dehiscence (eyetube.net/?v=ifosq).
LIMITATIONS
There are limitations with any technology. The biggest hurdles to incorporating laser-assisted cataract surgery (LACS) in a practice are expense and financing. This state-of-the art equipment is a costly investment, although many companies now offer extended payment options or rental programs. Recouping the investment can take time, particularly because treatment with LACS is not covered by insurance, and many patients simply do not have the extra income to take advantage of the procedure.
LACS is not an option for all patients—even for those are willing to pay for it. The laser has to dock with the eye near the limbus. Docking may be prevented (1) because the palpebral fissure is too small, (2) there is a prior surgical bleb from glaucoma surgery or a previously placed seton, or (3) scar tissue prevents transmission of the laser energy into the eye.
The laser only transmits through clear tissue; so patients who present with corneal scarring may not be ideal candidates for LACS. The laser treatment creates penetrating arcuate incisions in the cornea that produce gas, which could track along the prior incisions and open them. Patients who have had a corneal transplant or scarring from a radial keratotomy that could block the laser must be carefully evaluated for candidacy.
IN SUMMARY
Cataract surgery has continually improved, with new techniques, instruments, and technology. Combining some of the newest innovations can create synergy, allowing a safer and more predictable outcome. In my hands, use of a different phaco tip, in combination with femtosecond laser treatment and a variety of settings on the ultrasound/irrigation/aspiration apparatus, has allowed me to better handle both routine and difficult cases. As exemplified by the two cases I reported, surgeries that previously could turn into nightmares are now being completed without difficulty. I look forward to further changes in techniques, as the ophthalmic community pushes forward with new technology.
Subba R. Gollamudi, MD
• Medical Director and Managing Partner, Eye Specialty Group, Memphis, Tennesee
• drsubbagollamudi@esg.md
• Financial disclosure: Consultant, member of the speakers’ bureau (Abbott Medical Optics) Speaker (Alcon, Bausch + Lomb, ForTec Medical)

