Since the early 1990s, when the concepts of keratomileusis, the microkeratome, and the excimer laser were combined to create LASIK, more than 40 million procedures have been performed globally.1 During this time, huge advances have been made in the technologies and in our understanding of the procedure that have resulted in a quantum leap in safety, predictability, and efficacy—to the point where a patient has an extraordinarily high chance of ending up effectively free from the hassles of spectacles and contact lenses.
AT A GLANCE
- There is significant variability between patients in how the cornea reacts after laser refractive surgery, which can be explained only by variability in corneal biomechanics.
- Corneal biomechanics coupled with epithelial thickness mapping represents the richest area for significant innovation in corneal refractive surgery.
- Developing the ability to map biomechanical properties of the entire cornea in three dimensions in vivo, combined with finite element models validated by clinical studies, would open the prospect of truly customized corneal refractive surgery and provide another diagnostic method for keratoconus screening.
We can achieve refractive predictability to within ±0.50 D in about 80% of eyes and within ±1.00 D in almost all eyes with low to moderate myopia.2 This translates to making nearly all patients 20/20 or better and virtually every patient 20/40 or better, although many patients can achieve vision better than 20/20. We are now entering a new era in which we should be aiming to provide vision the same as or better than glasses, and we should not be satisfied with just achieving 20/20 on a 100% contrast Snellen chart.
In the past 25 years, we have seen the development and refinement of laser technology and of ablation profile designs, but there is now little scope left for significant improvements in outcomes from improved technology. The question, then, is how do we improve LASIK results from excellent to near-perfect? Aside from the limiting factor of measuring refractive error (which has a repeatability of ±0.25 D),3 the answers, in my opinion, lie with corneal biomechanics and epithelial dynamics. This article focuses on biomechanics and leaves epithelial dynamics for discussion at another time.
VARIABLE REACTION
There is significant variability among patients in how the cornea reacts after laser refractive surgery, and this can be explained only by variability in corneal biomechanics. For example, we see large scatter in the changes in higher-order aberrations after LASIK. Another example is IOP, which is reduced on average (as expected due to a reduction in corneal thickness) but actually increases in about 30% of eyes. The degree of postoperative change ranges from a 10 mm Hg increase to a 15 mm Hg decrease.4 Other studies have shown that corneal biomechanical properties change with age and are different between myopic and hyperopic eyes; the cornea tends to be stiffer in hyperopia.5
A deeper understanding of corneal biomechanics combined with a method of measuring corneal biomechanical properties accurately in vivo may be needed to bring on a second generation of custom ablation profiles. The difficulty is that understanding and measuring corneal biomechanics are both complex problems, so the final solution may be a while in coming. However, research in both areas is becoming more widespread.
UNDERSTANDING and MEASURING CORNEAL BIOMECHANICS
Understanding. In terms of understanding corneal biomechanics, a number of groups are working on finite element models of the cornea (and whole eye) with a view to being able to predict how an individual cornea will change following a specific procedure.6,7 This theoretical work continues to improve with the sophistication of the models, and also with the reliability of the biomechanical parameters provided by new measurement methods. For example, these models now include nonlinear elastic characteristics of the stroma based on data from studies showing that the anterior stroma has greater tensile strength than the posterior stroma. These differences are seen in cohesive tensile strength,8 tangential tensile strength,9 and transverse shear strength,10 all of which show extremely similar depth-dependent profiles. This nonlinearity has been explained by imaging of the 3-D distribution of collagen in the stroma, which showed the interwoven nature of collagen fibers in the anterior stroma compared with the posterior.11-13

Figure 1. The ORA is capable of measuring biomechanical properties in vivo.
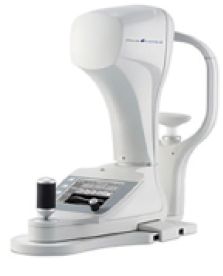
Figure 2. The Corvis ST is capable of measuring biomechanical properties in vivo.
Measuring. The great challenge, however, is measuring biomechanical properties in vivo in a regular clinical setting. In vivo measurements such as the Ocular Response Analyzer (Reichert Technologies; Figure 1)14 and Corvis ST (Oculus Optikgeräte; Figure 2)15 are providing the first insights into ocular biomechanics in terms of broad population differences, but the scatter in the measurements means that we are a long way from applying biomechanical information outside of diagnostics.
The other issue with these methods is that they provide values representing the global biomechanics but cannot provide localized information. For example, it has been shown using Brillouin microscopy that the biomechanical strength of a keratoconic cornea is different from that of a normal cornea only in the location of the cone.16 In other words, a keratoconic cornea is not necessarily inherently biomechanically weaker, it is only weaker in specific locations, leading to a stress concentration in that area and, hence, progression of the forward protrusion of the cone. Therefore, it is likely that a biomechanical map (rather than global parameters) will be required for use in screening for keratoconus and to act as a customized import into the finite element models.
OTHER APPROACHES TO UNDERSTANDING
Not all corneal biomechanical effects require such sophisticated analysis in order to be addressed. For example, tomographic and population regression analyses have been used to classify susceptibility to ectasia.17 That is, a biomechanically abnormal cornea can be identified by proxy using tomographic and other clinical data with high sensitivity and specificity.
Similarly, the major cause of night vision disturbances after laser refractive surgery, induced spherical aberration, has been understood and largely dealt with in the absence of biomechanical data. While spherical aberration could be partially explained by excimer laser fluence projection errors in peripheral ablation,18 the majority of the spherical aberration is due to corneal biomechanics. Using very–high-frequency digital ultrasound, we showed that, after an ablation, the peripheral stroma was thicker outside the zone of tissue ablation.19 This agrees with earlier reports of peripheral topographic changes outside the treatment zone after PTK20,21 and can be understood by considering that flap creation and stromal tissue ablation sever the anterior corneal lamellae, which means that the peripheral anterior lamellae are no longer under tension and, therefore, relax, spread out, and result in stromal thickening.22 It has been possible to develop ablation profiles with extended transition zones to precompensate for the expected peripheral expansion and reduce the induction of spherical aberration.23-25
ELIMINATING THE FLAP
Although we may have reached a plateau of technological improvement in excimer laser tissue ablation, the introduction of small incision lenticule extraction (ReLEx SMILE),26 a flapless form of keratomileusis, has changed the face of corneal refractive surgery in a number of ways, none more so than in its effect on corneal biomechanics, and, hence, on spherical aberration and optical quality.
In SMILE, due to the absence of a flap and the direct extraction of a stromal lenticule from within the body of the stroma through a keyhole 2-mm incision, the anterior-most stromal lamellae remain intact postoperatively, except in the region of the incision. This provides a biomechanical advantage, as the anterior region is the strongest part of the corneal stroma. By comparison, the anterior stromal lamellae are severed during LASIK and PRK—in LASIK by the creation of the flap and the excimer laser ablation, and in PRK by the excimer laser ablation. Therefore, SMILE reduces the tensile strength of the cornea less than LASIK or PRK do.
Whereas residual stromal thickness in LASIK is calculated as the amount of stromal tissue left under the flap, in SMILE, the equivalent value is calculated as the total uncut stroma (ie, the stroma above and below the lenticule). Moreover, given the decreasing strength of stroma with depth, this calculation can be extended to consideration of the tensile strength of the uncut stroma.
Case in Point
In an eye with central pachymetry of 588 μm, a 7-mm zone was used to treat -10.00 D (203-μm tissue removal) with a 135-μm SMILE cap thickness. The stromal thickness under the lenticule was 250 μm, but the total uncut stromal thickness was 335 μm, providing a postoperative tensile strength of 58%. By comparison, a -10.00 D LASIK treatment using a 6-mm optical zone with a 100-μm flap would leave a residual stromal thickness of 298 μm, representing a postoperative tensile strength of 44%. The spherical aberration induced was only 0.15 μm in the SMILE case, whereas it would be 0.75 μm in the LASIK case.
We have evaluated the effect of this phenomenon on safety in SMILE by developing a postoperative tensile strength calculator27 based on Randleman’s stromal tensile strength data.8 As an example, removing 100 µm of stroma via ablation (in LASIK or PRK) or as a lenticule (in SMILE) from a 550-µm thick cornea, the model calculated the postoperative tensile strength would be 75% of the initial value after SMILE performed with a 130-µm cap, 68% after PRK, and 54% after thin-flap (100-µm) LASIK.
We can take advantage of this difference in postoperative biomechanics to improve the optical quality of outcomes after SMILE by better controlling the induction of spherical aberration. Our studies have shown that the same amount of spherical aberration is induced by the spherical SMILE lenticule profile in a 6-mm zone as is by the aspherically optimized laser blended vision ablation profile,28 but with less tissue removal with the SMILE profile.29 Therefore, spherical aberration control can be improved in SMILE by increasing the optical zone, even if this means greater tissue removal, as the postoperative tensile strength is still greater than it would be by an equivalent LASIK treatment (see Case in Point).
SUMMARY
Corneal biomechanics and epithelial thickness mapping represent the richest areas for significant innovation in corneal refractive surgery. Developing the ability to map biomechanical properties of the entire cornea in three dimensions in vivo, combined with finite element models validated by clinical studies, would open the prospect of truly customized corneal refractive surgery, as well as provide another diagnostic method for keratoconus screening. The future is obvious, we just need to find a way to achieve it.
1. 2014 Global Refractive Marketing Report, Market Scope. August 2014: 10-11.
2. Reinstein DZ, Carp GI, Archer TJ, Gobbe M. Transitioning from mechanical microkeratome to femtosecond flap creation: comparing experienced vs novice LASIK surgeon visual outcomes for the first 200 myopic procedures. J Cataract Refract Surg. 2012;38:1788-1795.
3. Reinstein DZ, Yap TE, Carp GI, Archer TJ, Gobbe M. Reproducibility of manifest refraction between surgeons and optometrists in a clinical refractive surgery practice. J Cataract Refract Surg. 2014;40:450-459.
>4. Chang DH, Stulting RD. Change in intraocular pressure measurements after LASIK: the effect of the refractive correction and the lamellar flap. Ophthalmology. 2005;112:1009-1016.
5. Roberts CJ, Reinstein DZ, Archer TJ, Mahmoud AM, Gobbe M, Lee L. Comparison of ocular biomechanical response parameters in myopic and hyperopic eyes using dynamic bidirectional applanation analysis. J Cataract Refract Surg. 2014;40:929-936.
6. Sinha Roy A, Dupps Jr WJ, Roberts CJ. Comparison of biomechanical effects of small-incision lenticule extraction and laser in situ keratomileusis: finite-element analysis. J Cataract Refract Surg. 2014;40:971-980.
7. Studer HP, Riedwyl H, Amstutz CA, Hanson JV, Buchler P. Patient-specific finite-element simulation of the human cornea: a clinical validation study on cataract surgery. J Biomech. 2013;46:751-758.
8. Randleman JB, Dawson DG, Grossniklaus HE, McCarey BE, Edelhauser HF. Depth-dependent cohesive tensile strength in human donor corneas: implications for refractive surgery. J Refract Surg. 2008;24:S85-89.
9. Scarcelli G, Pineda R, Yun SH. Brillouin optical microscopy for corneal biomechanics. Invest Ophthalmol Vis Sci. 2012;53:185-190.
10. Petsche SJ, Chernyak D, Martiz J, Levenston ME, Pinsky PM. Depth-dependent transverse shear properties of the human corneal stroma. Invest Ophthalmol Vis Sci. 2012;53:873-880.
11. Winkler M, Shoa G, Xie Y, et al. Three-dimensional distribution of transverse collagen fibers in the anterior human corneal stroma. Invest Ophthalmol Vis Sci. 2013;54:7293-7301.
12. Winkler M, Chai D, Kriling S, et al. Nonlinear optical macroscopic assessment of 3-D corneal collagen organization and axial biomechanics. Invest Ophthalmol Vis Sci. 2011;52:8818-8827.
13. Morishige N, Takagi Y, Chikama T, Takahara A, Nishida T. Three-dimensional analysis of collagen lamellae in the anterior stroma of the human cornea visualized by second harmonic generation imaging microscopy. Invest Ophthalmol Vis Sci. 2011;52:911-915.
14. Luce DA. Determining in vivo biomechanical properties of the cornea with an ocular response analyzer. J Cataract Refract Surg. 2005;31:156-162.
15. Huseynova T, Waring GO 4th, Roberts C, Krueger RR, Tomita M. Corneal biomechanics as a function of intraocular pressure and pachymetry by dynamic infrared signal and Scheimpflug imaging analysis in normal eyes. Am J Ophthalmol. 2014;157:885-893.
16. Scarcelli G, Besner S, Pineda R, Yun SH. Biomechanical characterization of keratoconus corneas ex vivo with Brillouin microscopy. Invest Ophthalmol Vis Sci. 2014;55:4490-4495.
17. Ambrosio Jr R, Ramos I, Lopes B, et al. Assessing ectasia susceptibility prior to LASIK: the role of age and residual stromal bed (RSB) in conjunction to Belin-Ambrosio deviation index (BAD-D). Rev Bras Oftalmol. 2014;73:75-80.
18. Mrochen M, Seiler T. Influence of corneal curvature on calculation of ablation patterns used in photorefractive laser surgery. J Refract Surg. 2001;17:S584-587.
19. Reinstein DZ, Silverman RH, Raevsky T, et al. Arc-scanning very high-frequency digital ultrasound for 3D pachymetric mapping of the corneal epithelium and stroma in laser in situ keratomileusis. J Refract Surg. 2000;16:414-430.
20. Dupps WJ, Jr., Roberts C. Effect of acute biomechanical changes on corneal curvature after photokeratectomy. J Refract Surg. 2001;17:658-669.
21. Dupps WJ, Roberts C, Schoessler JP. Peripheral lamellar relaxation. Paper presented at: the Association for Research in Vision and Ophthalmology Annual Meeting; May 14-19, 1995; Fort Lauderdale, FL.
22. Roberts C. The cornea is not a piece of plastic. J Refract Surg. 2000;16:407-413.
23. Vinciguerra P, Camesasca FI, Urso R. Reduction of spherical aberration with the Nidek NAVEX customized ablation system. J Refract Surg. 2003;19:S195-201.
24. El Danasoury AM, Holladay J, Waring GO 3rd, Pieger S, Bains HS. A contralateral, randomized comparison of optimized prolate ablation and conventional LASIK for myopia with the NIDEK excimer laser platform. J Refract Surg. 2012;28:453-461.
25. Arba Mosquera S, Ewering T. New asymmetric centration strategy combining pupil and corneal vertex information for ablation procedures in refractive surgery: theoretical background. J Refract Surg. 2012;28:567-573.
26. Sekundo W, Kunert KS, Blum M. Small incision corneal refractive surgery using the small incision lenticule extraction (SMILE) procedure for the correction of myopia and myopic astigmatism: results of a 6 month prospective study. Br J Ophthalmol. 2011;95:335-339.
27. Reinstein DZ, Archer TJ, Randleman JB. Mathematical model to compare the relative tensile strength of the cornea after PRK, LASIK, and small incision lenticule extraction. J Refract Surg. 2013;29:454-460.
28. Srivannaboon S, Reinstein DZ, Archer TJ, Chansue E. Spherical aberration from myopic excimer laser ablation for aspheric and non-aspheric profiles. Optom Vis Sci. 2012;89:1211-1218.
29. Reinstein DZ, Archer TJ, Gobbe M. ReLEx SMILE induces significantly less spherical aberration than wavefront optimised sub-Bowman’s LASIK for any given residual postoperative relative tensile strength. Paper presented at: the Association for Research in Vision and Ophthalmology Annual Meeting; May 4-8, 2014; Orlando, FL.
Dan Z. Reinstein, MD, MA(Cantab), FRCSC, DABO, FRCOphth, FEBO
– Medical Director, London Vision Clinic
– Professor of Clinical Ophthalmology, Department of Ophthalmology, Columbia University Medical College, New York
– Professeur Associé, Centre Hospitalier National d’Ophtalmologie, Paris
– Financial disclosure: Consultant (Carl Zeiss Meditec), Financial interest (ArcScan)
– dzr@londonvisionclinic.com

