CXL is a promising method to treat keratoconus and corneal ectasia. The current standard procedure, the Dresden protocol, is widely used in clinics worldwide. However, great interest and effort are currently being devoted to developing improved procedures that require less time, have shorter postoperative downtime, and produce more efficient and reliable clinical outcomes.
A crucial determinant of the treatment outcome in CXL procedures is the degree of corneal rigidity conferred to the corneal stroma. In the quest to improve CXL procedures, many research groups and companies have been attempting to create measuring tools that can monitor corneal stiffness. In this context, we have developed an all-optical technique termed Brillouin microscopy.1
Brillouin microscopy is based on spectral analysis of light scattered from within corneal tissue. Within the cornea, the interaction between light and microscopic mechanical vibrations that are inherently present thermodynamically causes a small change in the light frequency, so the mechanical information can be measured optically. In the past several years, using Brillouin microscopy, we have measured age-related stiffening of the crystalline lens in mice in vivo2 and demonstrated mapping of corneal elasticity in animal and human tissue.3,4 Recently, Brillouin imaging provided novel insights into the biomechanical effect of keratoconus both ex vivo and in vivo.5,6
To investigate the utility of Brillouin microscopy in CXL, we imaged porcine corneas before and after riboflavin-assisted CXL performed using the Dresden protocol.7 A significant increase in corneal modulus was observed immediately after CXL (Figure 1). The increase of Brillouin modulus was depth-dependent, decreasing from anterior to posterior regions, indicating that the stiffening of the anterior corneal stroma contributes the most to mechanical outcomes.
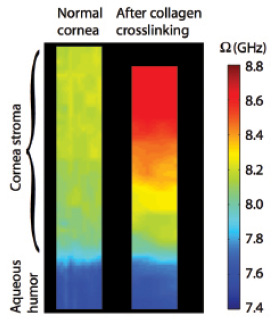
Figure 1. Brillouin images of normal porcine corneal tissue before and after standard epi-off CXL. Imaged area: 800 (z) X 50 μm (x).
We have proposed a corneal stiffening index (CSI) as a quantitative measure of the mechanical efficacy of a specific CXL procedure that allows direct comparison to the Dresden protocol. By definition, the CSI of the Dresden protocol is 100. Using this measure, we found that the CSI of epi-on CXL was 33. In other words, the procedure has one-third the mechanical efficacy of the Dresden protocol. We also noticed that postoperative dehydration had a significant mechanical effect, which suggests that the mechanical outcome of CXL should be evaluated when the corneal hydration has returned to baseline levels.
Brillouin microscopy could become a useful quantitative, high-resolution clinical tool for CXL.7,8 The dependence of the mechanical outcome on several operational parameters with and without epithelial debridement can be quantified. As we expect commercial instruments to be available in the near future, it is foreseeable that Brillouin technology may find widespread application in the clinic as a monitoring tool to assess and follow the mechanical outcomes of CXL treatment.
1. Scarcelli G, Yun SH. Confocal Brillouin microscopy for three-dimensional mechanical imaging. Nature Photonics. 2008;2:39-43.
2. Scarcelli G, Kim P, Yun S. In vivo measurement of age-related stiffening in the crystalline lens by Brillouin optical microscopy. Biophysical J. 2011;101:1539-1545.
3. Scarcelli G, Pineda R, Yun S. Brillouin optical microscopy for corneal biomechanics. Invest Ophthalmol Vis Sci. 2012;53:185-190.
4. Scarcelli G, Yun S. In vivo Brillouin optical microscopy of the human eye. Optics Express. 2012;20:9197-9202.
5. Scarcelli G, Besner S, Pineda R, Yun S. Biomechanical characterization of keratoconus corneas ex vivo with Brillouin microscopy. Invest Ophthalmol Vis Sci. 2014;55:4490-4495.
6. Scarcelli G, Besner S, Pineda R, Kalout P, Yun SH. In vivo biomechanical mapping of normal and keratoconus corneas. JAMA Ophthalmol. In press.
7. Scarcelli G, Kling S, Quijano E, Pineda R, Marcos S, Yun SH. Brillouin microscopy of collagen crosslinking: noncontact depth-dependent analysis of corneal elastic modulus. Invest Ophthalmol Vis Sci. 2013;54:1418-1425.
8. Cherfan D, Verter EE, Melki S, et al. Collagen cross-linking using rose bengal and green light to increase corneal stiffness. Invest Ophthalmol Vis Sci. 2013;54:3426-3433.
Giuliano Scarcelli, PhD
- The Fischell Department of Bioengineering, University of Maryland, College Park
- Harvard Medical School and Wellman Center for Photomedicine, Massachusetts General Hospital, Cambridge, Massachusetts
- scarc@umd.edu
- Financial disclosure: Patents related to Brillouin technology (Massachusetts General Hospital)
Seok Hyun Yun, PhD
- Harvard Medical School and Wellman Center for Photomedicine, Massachusetts General Hospital, Cambridge, Massachusetts
- Harvard-MIT Health Sciences and Technology, Cambridge, Massachusetts
- syun@hms.harvard.edu
- Financial disclosure: Patents related to Brillouin technology (Massachusetts General Hospital)

