Today, applications of teleophthalmology take multiple forms: providing access to eye specialists for patients in remote areas; allowing ophthalmic disease screening, diagnosis, and monitoring over any distance; and even supporting distant learning. None of this would be possible, however, without the enabling technology. As rapid innovations in the tech world continue to arise, devices are being developed and upgraded specifically to facilitate the practice of teleophthalmology. Of primary importance are the capture and transfer of clinical images and video. Below is an overview of several devices that are enhancing how users obtain, store, and send visual data to provide improved patient care anywhere in the world.
D-Eye
The D-Eye Portable Retinal Imaging System (Figure 1A) attaches to a smartphone, creating a modern-day ophthalmoscope capable of recording and transmitting high-definition videos and still images for clinical assessment. The lens attaches to the smartphone via a specially designed, lightweight magnetic bumper attachment. By using the smartphone camera focus feature, aiming at the retina, and approaching the cornea to 1 cm of distance, vivid videos can be recorded and saved to the D-Eye ImageVault, a secure, cloud-based patient record system, for further assessment and long-term storage for patient history.
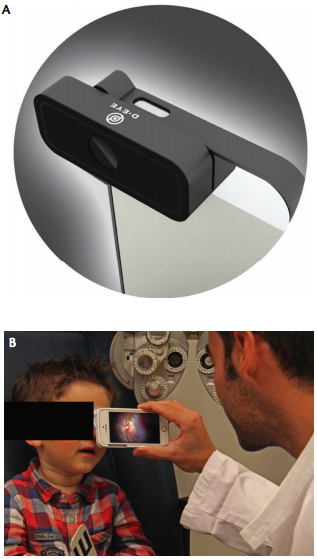
Figure 1. The D-Eye lens connected to a smartphone (A). D-Eye is used to image a pediatric patient (B).
D-Eye can be used to conduct routine eye exams and retina screenings for detection of a variety of disorders.1 Users can see the optic nerve head without use of dilating drops, look for neurologic disorders associated with the eye, record images of children and infants without dilation (Figure 1B), examine bed-ridden patients, perform emergency room evaluations, and review before-and-after treatment images with patients or family members. Major pathologies that can be seen with D-Eye include glaucoma, intermediate-stage diabetic retinopathy, and age-related macular degeneration.
D-Eye can be used on dilated or undilated eyes. When the pupil is dilated, the D-Eye lens captures a field of view of approximately 20° in a single fundus image. According to the company, videos allow the user to angle the lens to capture more of the outer edges of the retina than still photos. In video mode, an acquisition protocol would allow the user to pan the retina, starting from the posterior pole and moving to the peripheral retina and the equator. Color digital images and videos of the retina can be obtained, encompassing the entire posterior pole, including the macula, optic disc, and peripheral retina.
D-Eye is portable, requiring no external power or lighting, and is noninvasive and ergonomic. Users can record multiple high-definition images or videos and store information in a built-in patient file. D-Eye images and videos can also be stored in a private and secure cloud-based system.
D-Eye is available in a model designed for veterinary use in animal eyes.
1. D-Eye. https://www.D-Eyecare.com/. Accessed May 22, 2016.
visoClip AND visoScope
Recognizing challenges associated with the purchase and portability of fundus cameras in developing countries, oDocs Eye Care sought to develop a retinal imaging device that was accurate, accessible, and affordable.1 The company developed the visoClip and visoScope (Figure 2) to help users transform their iPhones into anterior segment and retinal cameras.

Figure 2. The visoClip anterior segment imaging adapter (A). The visoScope retinal imaging adapter (B).
D-Eye
The visoClip anterior segment imaging adapter clips onto an iPhone and transforms it into an anterior segment microscope, capable of up to 10X optical magnification. Users can quickly capture high-resolution photos and videos using focused, angled illumination. The visoClip can be used to visualize acute corneal lesions and is ideal for referrals, according to company literature.1
The visoScope retinal imaging adapter adds retinal imaging capability to the iPhone when a direct ophthalmoscope is not available, the company says.1 The specialized optics and high-quality antireflective crown lens provides a 50° field of view, comparable to that of a conventional fundus camera.
The corresponding oDocs app features a range of eye tests.
1. oDocs Eye Care. http://www.odocs-tech.com/#products. Accessed May 24, 2016.
Teleophthalmology in the ER
1. Wedekind L, Sainani K, Pershing S. Supply and perceived demand for teleophthalmology in triage and consultations in California emergency departments. JAMA Ophthalmol. 2016;134(5):537-543.
PEEK
The Portable Eye Examination Kit (Peek; Peek Vision) is a mobile phone–based ophthalmic testing system developed to perform comprehensive eye exams (Figure 3). Shortages in ophthalmic personnel, high costs, and difficulty transporting equipment have made it challenging to offer eye care in many rural areas.1 According to the company, Peek offers a solution to overcome barriers of limited access to traditional ophthalmic testing methods. It has been pilot-tested on adults in Nakuru, Kenya.1

Figure 3. Retinal imaging is performed with Peek.
Used with the Peek app, Peek Retina combines a traditional ophthalmoscope and a retinal camera in a mobile phone, providing a portable, affordable, and user-friendly way to carry out comprehensive eye exams. The high quality of the images enables users to view cataracts clearly enough for treatment classification and to detect signs of glaucoma, macular degeneration, diabetic retinopathy, and signs of nerve disease, according to company literature.2
The Peek vision test is based on one letter: a tumbling-E shape, making it simple for patients to recognize. The tumbling E does not rely on an individual knowing the English language, yet this test has been shown to give the same results as traditional visual acuity tests, according to the company. The patient uses his or her finger to indicate how he or she thinks the E is positioned. With Peek SightSim, users can see a live simulation of how a patient sees the world compared with those who have normal vision.
Images and patient information can be securely stored in and shared from the Peek app for off-site review. Whether Peek is being used to transfer information between practitioners or from a remotely based health worker to a treatment clinic, all images are available to send whenever the phone has a data or Wi-Fi connection so that diagnoses can be carried out by a trained eye care specialist.
The company is currently evaluating tests it has developed for color blindness and for contrast sensitivity.
1. Lodhia V, Karanja S, Lees S, Bastawrous A. Acceptability, usability, and views on deployment of Peek, a mobile phone mHealth intervention for eye care in Kenya: qualitative study. JMIR mHealth and uHealth. 2016;4(2):e30.
2. What it Does. Peek Vision website. http://www.peekvision.org/what-it-does. Accessed May 22, 2016.

