
As little as 6 years ago, a lack of treatment options led many eye care providers to ignore patient complaints about dry, scratchy eyes and focus on issues that they could address. Today, providers have more options to treat dry eye disease (DED), and patients might seek out your competitors for services that your practice does not offer.
DED care is not difficult—it involves paying attention to the details. See the signs, listen to patients explain their symptoms, and address the issue. The following seven steps can help make DED care a reality in your practice.
STEP no. 1: IDENTIFY YOURSELF
What do you want your practice to be, and how does that compare with what it is now? Does everyone at your practice agree with the decision to offer DED care? This is important regardless of the size of your practice. Everyone must be on board with the decision, or your success will be limited. Remember, patients discuss their care with other members of your staff, so they should hear a consistent message.
Once you decide to proceed, determine if there is a single person within your organization who can be the dry eye specialist, or if the role will be shared by all practice providers. If you go with a single specialist, give that person the power to make treatment decisions. I also recommend appointing a staff champion who will help with implementation.

Figure. Educational events can help your team to understand DED and get them up to speed on the latest technologies.
STEP no. 2: EDUCATE YOUR TEAM
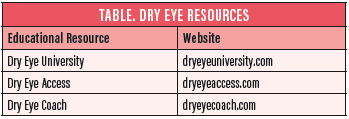
Provide appropriate educational resources to help your team understand DED and get all team members up to speed on the latest technologies. This can be done with various online resources, such as those in the Table below, and by hosting and attending educational events (Figure). Recognizing the value of a multifaceted approach is important. I often encounter practices that invest in only one technology or try only one product, as if it is the answer for all patients with DED. Not all patients are the same, and neither are their symptoms.
When your practice is close to rolling out its DED services, it will be important to hold a staff meeting and provide group education. Take advantage of the hands-on training that vendors offer for their products.
STEP no. 3: DEVELOP A DED STANDARD OF CARE
In the field of glaucoma, as an example, guidelines stipulate how often eye care providers should perform visual field testing and advanced imaging, the frequency of follow-up appointments, and when surgery is indicated. These standards are based on factors such as the patient’s age and the severity of disease, with the goal of slowing disease progression. Similarly, physicians should be focused on slowing the progression of DED. By learning how to spot the early signs of DED and developing standards for its diagnosis and management, you will help patients maintain a healthy ocular surface.
STEP no. 4: IDENTIFY YOUR PATIENTS
You do not need an advertising campaign to identify patients with DED. You will examine patients for other conditions as a part of your normal daily schedule, and many will have signs and symptoms of DED if you look for them. Consider utilizing the Standardized Patient Evaluation of Eye Dryness (SPEED) questionnaire to identify patients with DED.
STEP no. 5: FOCUS ON FLOW
One concern for providers who hesitate to offer DED treatment is that they do not want to mess up patient flow, efficiency, or productivity in the practice. When adding DED services to your practice’s offering, it is important to consider several questions, outlined here.
Will you treat DED patients upon identification, or will you bring them back for another appointment? (I recommend the former.) Administer the SPEED questionnaire at intake, and design the initiation of treatment around the SPEED score.
Patients with severe DED will leave the practice with prescriptions and products and have a future procedure scheduled. Patients whose SPEED score indicates mild or moderate DED may leave with some products to try before a return appointment, at which time they will undergo diagnostic testing to form a treatment plan.
If you prefer instead to bring identified DED patients back for another appointment, I advise caution. It is possible that these patients have been describing their symptoms for years, and they believe no one has listened to them. Patients tend to have a high no-show rate when you dismiss symptoms and put treatment off until the next visit. Patients want what is important to them to be important to you.
I also advise against block scheduling. It is unlikely that you could manage the volume of DED patients that your practice will have in a short time. Your practice could start with this approach, but it is likely that the block will be booked out for weeks, if not months.
Where will diagnostic testing equipment be located in the clinic? Who will perform those tests? At what point in the examination will you introduce patients to their treatment options? These are all questions you should answer at the outset of planning for your DED services so that everyone in the practice is on the same page.
Who will counsel patients? Contact lens counselors, surgical counselors, and refractive surgery coordinators are generally all great educators, and education consumes one of the biggest chunks of time in DED treatment. The more a patient knows before seeing the doctor, the more efficient and successful the appointment will be. Your practice may also want to create tutorials or use software to help educate patients.
STEP no. 6: SET A BUDGET
Create a budget based on your standard of care. What does your practice require to meet the needs of its DED patients? Ideally, your standard of care will include products, services, procedures, and prescribed medications and devices.
Also, set your pricing for products and services. Verify coverage with your carriers on all services and script financial discussions with patients about the noncovered services.
Once your budget is clear, start meeting with vendors in the DED space to negotiate pricing and the acquisition of equipment and products.
STEP no. 7: GET STARTED
Start seeing patients. Once you are ready to roll out your DED offerings, patients will like having their DED-related concerns sympathetically heard by your team, and they will be excited to learn about the new treatment options that your practice offers.
CONCLUSION
DED care in your practice will become routine. Just give it time and focus on consistently applying the standards you designed for your practice. Tweak your presentations, attend meetings and webinars, and become the leading DED caregiver in your market.



