

Cataract surgeons frequently and comfortably assume various operating positions in response to their surgical preference, patient positioning, and the patient’s relative astigmatism. Modern operating chairs are of great help in this regard. Unfortunately, these accommodations are not always suitable. The Trendelenburg position,1,2 for example, can make it difficult for the surgeon to fit his or her legs under the operating table, and case reports have described cataract surgeons standing or operating face to face while the patient is seated.1,3,4
As the global population ages, the number of patients presenting for cataract surgery who have medical and social comorbidities will grow, and surgeons will need greater flexibility and creativity to cope with the demand. This article shares such a scenario and describes a technique for operating through a nasal incision from the contralateral side in order to overcome difficult patient positioning.
CASE PRESENTATION
A 68-year-old woman with a background of cognitive impairment, bipolar affective disorder, and advanced kyphoscoliosis presented for a cataract surgery evaluation. The patient’s preoperative visual acuity was impossible to quantify, and the examination was limited to brief visualization using a portable slit lamp. Her family stated that the patient could no longer read or watch television and that she only recognized the presence of family members when they spoke. Her family and surgeon decided that it was in the patient’s best interest to proceed with an examination under general anesthesia, followed by cataract surgery if appropriate. The surgeon expected to carry out the cataract procedure via a conventional approach once the patient was positioned under anesthesia.
SURGICAL APPROACH
On the day of surgery, the operating and anesthetic teams could not achieve the optimal supine position for the patient. Instead, she remained fixed in a flexed and rotated position (Figure 1), meaning that her right eye was inaccessible and her left eye was positioned such that superior and temporal access was impossible. A temporal approach was steep, which would have left much of the cornea covered by the narrow temporal palpebral aperture once the eye was in primary position. After considering the patient’s relatively flat nasal bridge, the teams determined that the safest access was across her nose from the contralateral side (Figure 2).
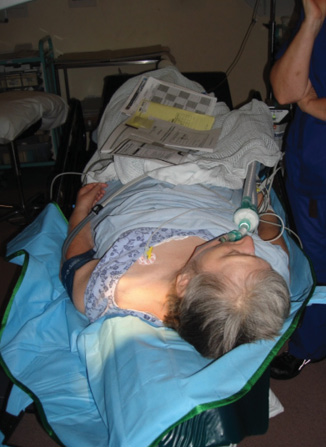
Figure 1. Rotated and flexed positioning associated with kyphoscoliosis.
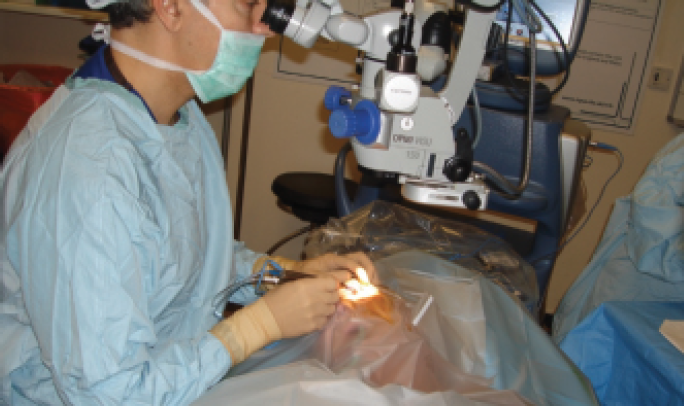
Figure 2. The surgeon operated across the patient’s nasal bridge to perform phacoemulsification on the left eye from the contralateral side.
Biometry using the A-scan and handheld keratometer was accomplished on the table, and the surgeon was able to successfully complete routine phacoemulsification and IOL implantation in the patient’s left eye. He placed a precautionary 10-0 polyglactin suture at the main incision in anticipation of potential difficulty with the patient’s postoperative care. Examination under anesthesia confirmed normal retinal and optic nerve anatomy. The patient received a prescription for routine postoperative topical antibiotic and steroid medication.
One week after surgery, the patient’s recovery was excellent, and her family reported a dramatic improvement in her visual ability.
CONCLUSION
In cases of extreme positioning difficulty, not only may a conventional approach to cataract surgery be unsuitable, but it may actually increase the risk of complications. Ophthalmologists have developed a variety of positioning strategies for these challenging scenarios. Operating through a nasal incision from the contralateral side is a newly described option.
1. Lee RM, Jehle T, Eke T. Face-to-face upright seated positioning for cataract surgery in patients who cannot lie flat. J Cataract Refract Surg. 2011;37(5):805-809.
2. Jensen LE, Muthialu A, Oetting TA. Kyphotic patient presents for cataract surgery: a systems based case. University of Iowa Health Care. http://www.EyeRounds.org/cases/90-Positioning-Patient-Kyphosis-Systems.htm. December 8, 2008. Accessed May 17, 2018.
3. Pajaujis M, Injarie A, Eke T. Extreme face-to-face positioning for cataract surgery with patient seated upright in motorized wheelchair. J Cataract Refract Surg. 2013;39(5):804-805.
4. Sharma V, Pandey SK. Phacoemulsification in postural disorders. Cataract & Refractive Surgery Today. April 2016;16(4):92-94. http://bit.ly/0718cabourne.



