
Life happens on small and grand scales, right in front of us and from afar; most of us want to experience all of it. Since the first bifocal IOLs were developed in the 1980s, scientists and manufacturers have been on a dedicated mission to provide individuals with great vision at all distances after cataract surgery.
AT A GLANCE
• Extended depth of focus technologies aim to increase overall depth of field.
• A small aperture or pinhole effect is one method of achieving extended depth of focus.
• An IOL using this approach has provided improved near, intermediate, and distance UCVA in patients.
Following those early bifocal lenses, the development of multifocal lenses provided good vision at multiple distances, and accommodative IOLs attempted to mimic the focusing ability of the natural eye. However, although many of these options have been successful in achieving good visual acuity at distinct distances, this has often come at the price of decreased overall quality of vision.1-3
Rather than creating two or three focal points, extended depth of focus (EDOF) technologies aim to increase overall depth of field, creating a fluid visual experience that provides better near vision than monofocal technologies and, at the same time, less trouble with glare and halos than multifocal IOLs. There are a number of EDOF lenses on the market, and they achieve their desired visual range via a variety of methods. The Symfony IOL (Abbott Medical Optics) has a unique echelette design. (The manufacturer refers to this lens as providing an extended range of vision, as opposed to EDOF.) The Light Adjustable Lens (Calhoun Vision) can be shaped to provide additional spherical aberration through postoperative irradiation of the silicone material with ultraviolet light.4
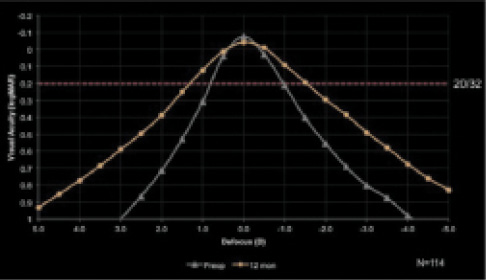
Figure 1. Comparison of patient defocus curves in an untreated presbyopic eye and an eye 1 year after Kamra implantation.
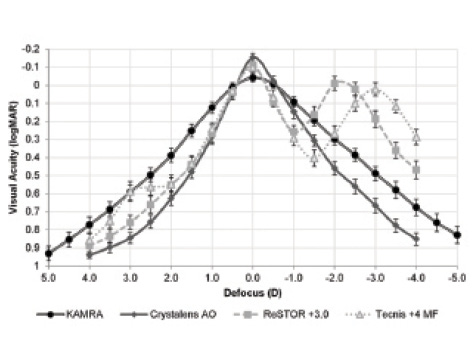
Figure 2. Monocular defocus curves show visual acuity (logMAR) versus defocus lens power at 6 months after Kamra inlay or presbyopia-correcting IOL implantation.
SMALL-APERTURE APPROACH
Another approach to EDOF is used in the IC-8 IOL (AcuFocus), a lens adaptation of the Kamra corneal inlay (AcuFocus) for presbyopia. This one-piece hydrophobic acrylic IOL has a centrally located opaque annular mask measuring 3.23 mm in total diameter with a 1.36-mm central aperture. The IC-8 IOL provides EDOF using the pinhole effect, blocking unfocused peripheral light rays and isolating more focused central and paracentral rays through the central aperture. The IOL mask is 15% smaller in diameter than the one used in the Kamra inlay to account for its more posterior placement. It also has fewer microperforations.
Investigators collected data from more than 20,000 patients worldwide with the Kamra inlay. They found that patients with the inlay gained a mean 3 lines of near visual acuity and 1 line of intermediate visual acuity, with a decrease of only 0.5 lines of monocular distance acuity and no decrease of binocular distance acuity.5 Results with the Kamra inlay remained stable over 60 months, even as presbyopia progressed.
In an eye with plano refraction, the small-aperture technique can provide an increased range of vision of about 2.5 D. If that is combined with slight myopia (-0.75 D), a patient can achieve a continuous functional range of vision of up to 3.5 D (Figure 1). When the Kamra inlay was compared against three presbyopia-correcting IOLs, it performed well at all distances, providing continuous functional vision across a large dioptric range (Figure 2).5
Contrast sensitivity is an important aspect of quality of vision and EDOF. In a comparison of patients implanted with the Kamra inlay or with one of three presbyopia-correcting IOLs, patients with the inlay had better contrast sensitivity than patients with multifocal IOLs. Patients also had significantly better binocular contrast sensitivity when compared with both those with either multifocal IOLs or accommodating IOLs.5
Available EDOF Technologies
• IC-8 IOL (AcuFocus)
• Hoya
• Light Adjustable Lens (Calhoun Vision)
• MiniWell (Sifi Medtech)
• RevIOL Tri-ED (VSY)
• Symfony IOL (Abbott Medical Optics)
INVESTIGATING SMALL-APERTURE EFFECTS
Using a binocular adaptive optics instrument, we simulated the effect of the small-aperture inlay and demonstrated a significant increment in depth of focus.6 There was a benefit in stereoacuity. We also compared stereo vision with two methods of presbyopia correction—monoviosion and the small-aperture effect—and found that although monovision correction reduced stereoacuity, the small aperture preserved it at nearly normal values.7
Because small-aperture devices function by eliminating some peripheral rays of light, we thought it important to evaluate how placement of the small-aperture mask affects visual performance. Using an eye model, we determined that, in eyes with little astigmatism and low aberrations, the optimum centration of the small aperture was near the corneal reflex position.8
Another important issue related to the small aperture is possible reduction of luminance. In that context, we recently analyzed the visual effect of the Stiles-Crawford (SC) peak decentration in patients with small apertures.9 The SC effect produces a change in the apparent brightness of rays entering the eye through different pupil positions. The SC peak is typically located 0.33 mm nasal to the pupil center, but it can be significantly more decentered in some patients. The small aperture is typically centered on the pupil or on the first Purkinje image.
My colleagues and I evaluated the impact of the SC peak location on the visual performance of eyes with a small aperture. We found that the quality of the retinal image in eyes with a small aperture was not affected by the location of the SC peak in most patients. Only in cases in which the SC peak was decentered by more than 2 mm was there a reduction in mesopic visual acuity. This suggests that centration of a small-aperture inlay or IOL is not a critical issue.
CONCLUSIONS
The IC-8 lens received the CE Mark, but the manufacturer is conducting a postapproval study in 12 centers in Europe to refine the procedure. The lens is implanted monocularly, and an IOL of the surgeon’s choice is used in the other eye.
A recent report found that 12 cataract patients who were implanted monocularly with the IC-8 lens showed significant improvement in distance, intermediate, and near visual acuity.10 At 12 months, mean monocular near, intermediate, and distance UCVA improved significantly in these patients, from J6 to J2 (P = .0051), from 20/44 to 20/21 (P = .0051), and from 20/32 to 20/20 (P = .001), respectively. All eyes maintained 20/40 or better visual acuity over a range of +0.50 D to -1.50 D of defocus, while patients perceived only a small magnitude of visual symptoms that they rated on the low end of a severity scale.10
The EDOF lens category sits in the treatment toolbox between monofocal and multifocal IOLs. These lenses can be used in patients without retinal disease who would not be happy with standard diffractive multifocal IOLs but who desire some spectacle independence. These lenses are filling a previously unmet need and providing many patients with an option for good quality of vision at a range of distances.
1. Davison JA, Simpson MJ. History and development of the apodized diffractive intraocular lens. J Cataract Refract Surg. 2006;32(5):849-858.
2. Bellucci R. Multifocal intraocular lenses. Curr Opin Ophthalmol. 2005;16(1):33-37.
3. Pepose JS, Wang D, Altmann GE. Comparison of through-focus image sharpness across five presbyopia-correcting intraocular lenses. Am J Ophthalmol. 2012;154(1):20-28.
4. Villegas EA, Alcón E, Mirabet S, Yago I, Marín JM, Artal P. Extended depth of focus with induced spherical aberration in light-adjustable intraocular lenses. Am J Ophthalmol. 2014;157(1):142-149.
5. Vilupuru S, Lin L, Pepose JS. Comparison of contrast sensitivity and through focus in small-aperture inlay, accommodating intraocular lens, or multifocal intraocular lens subjects. Am J Ophthalmol. 2015;160(1):150-162.
6. Tabernero J, Schwarz C, Fernández EJ, Artal P. Binocular visual simulation of a corneal inlay to increase depth of focus. Invest Ophthalmol Vis Sci. 2011;52:5273-5277.
7. Fernández EJ, Schwarz C, Prieto PM, Manzanera S, Artal P. Impact on stereo-acuity of two presbyopia correction approaches: monovision and small aperture inlay. Biomed Opt Express. 2013;4:822-830.
8. Tabernero J, Artal P. Optical modeling of a corneal inlay in real eyes to increase depth of focus: optimum centration and residual defocus. J Cataract Refract Surg. 2012;38:270-277.
9. Artal P, Prieto P, Robles C, Manzanera S, Holladay J. Visual effect of the Stiles-Crawford peak location in patients with a small-aperture corneal inlay. Paper presented at: European Society of Cataract and Refractive Surgeons Annual Meeting; September 5-9, 2015; Barcelona, Spain.
10. Grabner G, Ang R, Vilupuru S. The small aperture IC-8 intraocular lens, a new concept for added depth of focus in cataract patients. Am J Ophthalmol. 2015;160(6):1176-1184.e1.
Pablo Artal, PhD
•Professor, Laboratorio de Óptica, Universidad de Murcia, Spain
• pablo@um.es
• Financial disclosure: Consultant (AcuFocus)

