
In Western Europe, an estimated 3.2 million cataract surgeries are performed each year.1 Among individuals diagnosed with cataracts, around 9% have a coexisting diagnosis of glaucoma.2 With these numbers only increasing as the population ages, cataract surgeons are frequently faced with patients presenting with concomitant cataract and glaucoma.
AT A GLANCE
- Many surgeons view cataract surgery itself as a glaucoma procedure because it has IOP-lowering effects.
- Factors such as the number of medications a patient with glaucoma is taking, the stage of his or her disease, and the current and target IOPs should be considered when determining whether to combine cataract surgery with another procedure to lower IOP.
- With a phaco-plus procedure, the surgeon must consider whether to use a MIGS approach or a more invasive glaucoma surgical procedure.
Many surgeons view cataract surgery itself as a glaucoma procedure because it has IOP-lowering effects. A number of studies have shown that phacoemulsification can lower IOP,3 and strong evidence indicates that phacoemulsification is a better and safer treatment than either peripheral iridotomy or phacotrabeculectomy.4-6 For patients with concomitant cataract and glaucoma, the reduction in IOP seen after cataract surgery is an added benefit that may offer better postoperative IOP control than these other procedures.3 Should IOP reduction after cataract surgery be insufficient, topical therapy may be augmented or initiated, and laser trabeculoplasty or frank filtration surgery may be warranted. With that said, cataract surgery can result in an increase in IOP postoperatively in some patients. It is, therefore, vital to choose appropriate patients for standalone and combined procedures. In this article and in the accompanying graphic, I outline how and when I select cataract surgery alone or in combination with other procedures to control IOP in glaucoma patients.
WHEN IS CATARACT SURGERY ALONE SUFFICIENT?
Cataract surgery can be effective in lowering IOP, particularly in patients with angle-closure glaucoma (ACG).3 A recent review of the literature by the AAO assessed the effect of cataract surgery on IOP.7 The authors found that patients with ACG experienced a 30% reduction in IOP and a 58% reduction in the number of glaucoma medications needed after phacoemulsification. Patients with other forms of glaucoma who have little or no optic disc damage or visual field defects, and whose IOP is adequately controlled on medications, can also do well with standalone cataract surgery.
However, the efficacy of using phacoemulsification to reduce IOP in open-angle glaucoma (OAG) patients is more controversial. The same AAO report found that patients with OAG experienced significantly smaller benefits than those seen in patients with ACG, with only a 13% reduction of IOP and 12% reduction in number of medications.7 Two randomized controlled trials did demonstrate significant IOP reductions after cataract surgery; however, both had methodologic issues, including small sample sizes and the inclusion of no untreated control groups and no true glaucoma patients.8,9
Conversely, a prospective study of 63 patients in Japan demonstrated that patients with OAG undergoing phacoemulsification tended to have an increase in IOP postoperatively.10 In that trial, 13% of OAG patients had IOP spikes to greater than 30 mm Hg postoperatively, whereas no patients in a control group experienced spikes. However, as higher preoperative IOP appears to be proportional with higher postoperative IOP, preoperative IOP levels may be used as a predictor for postoperative outcomes.10,11
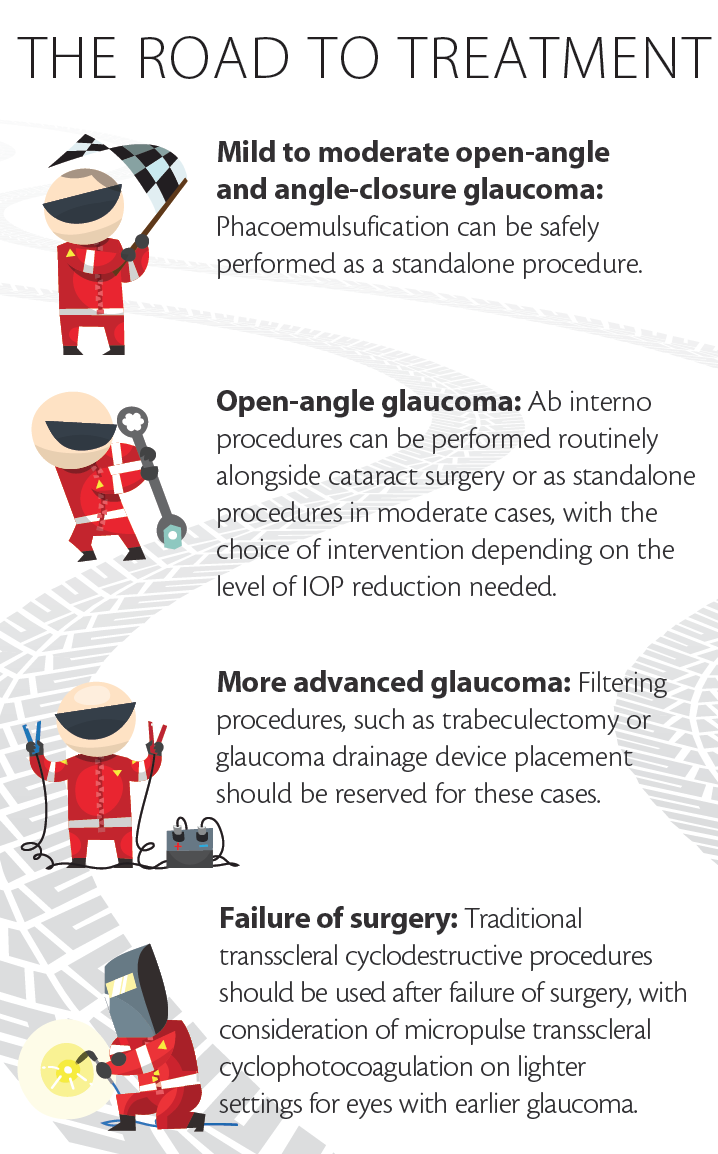
WHEN TO COMBINE WITH OTHER PROCEDURES
When it comes time for cataract surgery, some glaucoma patients need more than phacoemulsification alone to help control the chronic disease. These include patients with moderate or advanced glaucoma who have uncontrolled IOP despite using several medications and having undergone previous trabeculoplasty. These patients likely have an outflow facility compromise either in or distal to the trabecular meshwork.
Such patients may benefit from a phaco-plus procedure. Phaco-plus is a term describing a combined procedure: either cataract surgery plus microinvasive invasive glaucoma surgery (MIGS) or cataract surgery plus penetrating filtration surgery. Patients with significant disc and visual field damage and with borderline or uncontrolled IOP may benefit from a combined procedure.
If a patient’s IOP is borderline or above target pressure and the patient has mild to moderate glaucoma with mild to moderate visual field defects, that patient needs to achieve a postoperative IOP in the mid-teen range and would benefit from phacoemulsification plus MIGS. MIGS procedures include iStent implantation (Glaukos), trabeculotomy with the Trabectome (NeoMedix), endocyclophotocoagulation, implantation of a Xen gel stent (Allergan), ab interno canaloplasty performed with the iTrack illuminated microcatheter (Ellex), or goniotomy with the Kahook Dual Blade (New World Medical).
As the risk associated with MIGS is low and many MIGS procedures were conceived to be performed in combination with cataract surgery, I typically offer this phaco-plus option for patients who have mild to moderate glaucoma. This generally reduces IOP to the middle to lower teens and often eliminates or reduced the number of medications needed, even for patients with unstable pressures, without adding risk to the procedure.
Patients with moderate to advanced glaucoma despite two or more medications need to achieve a target IOP in the lower teens, which requires phacoemulsification plus a more involved procedure such as trabeculectomy or CO2 laser-assisted sclerectomy surgery (CLASS) with the IOPtiMate CO2 laser system (IOPtima). The nonpenetrating CLASS procedure has been shown to be safer and more effective than other nonpenetrating glaucoma procedures. It provides IOP control similar to that of trabeculectomy,12-14 and it can be performed by cataract and glaucoma surgeons as a standalone procedure or in combination with phacoemulsification. CLASS is appropriate for use in patients with primary OAG and pseudoexfoliative glaucoma.
In CLASS, similar to trabeculectomy, the surgeon performs a peritomy and creates a small scleral flap. The Schlemm canal is then essentially unroofed as the laser thins the scleral wall above the canal, which allows aqueous percolation to reduce IOP. The CO2 laser energy is absorbed by the percolating aqueous humor, preventing its penetration into the eye. This self-regulating safety mechanism, along with the absence of shunts, tubes, and other foreign bodies, reduces the risk of complications compared with other procedures.
If the patient’s target IOP range has not been reached by 6 weeks after the CLASS procedure, the surgeon can perform another simple procedure such as Nd:YAG laser goniopuncture in order to try to reach the target IOP.
CONCLUSION
In any patient with coexisting glaucoma and cataract, factors such as the number of medications the patient is taking, the stage of the patient’s disease, and the patient’s current IOP level and target IOP should be considered. With this knowledge, the surgeon can more clearly determine whether or not combined surgery is required at the time of cataract extraction. If a combined, phaco-plus procedure is decided upon, the surgeon must further consider whether to use a MIGS approach or a more invasive glaucoma surgical procedure.
1. Market Scope. https://market-scope.com/pressrelease/eu-5-ophthalmic-market-to-grow-more-than-5-percent-through-2021/
2. Tseng VL, Yu F, Lum F, Coleman AL. Risk of fractures following cataract surgery in Medicare beneficiaries. JAMA. 2012;308:493-501.
3. Brown RH, Zhong L, Lynch MG. Lens-based glaucoma surgery: using cataract surgery to reduce intraocular pressure. J Cataract Refract Surg. 2014;40:1255-1262.
4. Lam DS, Leung DY, Leung DY, et al. Randomized trial of early phacoemulsification versus peripheral iridotomy to prevent intraocular pressure rise after acute primary angle closure. Ophthalmology. 2008;115:1134-1140.
5. Azuara-Blanco A, Burr J, Ramsay C, et al; EAGLE study group. Effectiveness of early lens extraction for the treatment of primary angle-closure glaucoma (EAGLE): a randomised controlled trial. Lancet. 2016;388(10052):1389-1397.
6. Tham CC, Kwong YY, Leung DY, et al. Phacoemulsification versus combined phacotrabeculectomy in medically uncontrolled chronic angle closure glaucoma with cataracts. Ophthalmology. 2009;116:725-731.
7. Chen P, Lin S, Junk A, Radhakrishnan S, Singh K, Chen T. The effect of phacoemulsification on intraocular pressure in glaucoma patients: a report by the American Academy of Ophthalmology. Ophthalmology. 2015;122(7):1294-1307.
8. Samuelson TW, Katz LJ, Wells JM, Duh Y-J, Giamporcaro JE; for the US iStent Study Group. Randomized evaluation of the trabecular micro-bypass stent with phacoemulsification in patients with glaucoma and cataract. Ophthalmology. 2011;118:459-467.
9. Mansberger SL, Gordon MO, Jampel H, et al; for the Ocular Hypertension Treatment Study Group. Reduction in intraocular pressure after cataract extraction: the Ocular Hypertension Treatment Study. Ophthalmology 2012;119:1826-1831.
10. Yasutani H, Hayashi K, Hayashi H, Hayashi F. Intraocular pressure rise after phacoemulsification surgery in glaucoma patients. J Cataract Refract Surg. 2004;30(6):1219-1224.
11. Poley BJ, Lindstrom RL, Samuelson TW, Schulze R Jr. Intraocular pressure reduction after phacoemulsification with intraocular lens implantation in glaucomatous and nonglaucmoatous eyes; evaluation of a causal relationship between the natural lens and open-angle glaucoma. J Cataract Refract Surg. 2009;35:1946-1955.
12. Geffen N, Ton Y, Muñoz G, Mariotti C, Assia EI. CO2 laser-assisted sclerectomy surgery for open-angle glaucoma. European Ophthalmic Review. 2012;6(1):12-16.
13. Melamed S. CLASS procedure offers alternative treatment for glaucoma. Ocular Surgery News Europe Edition. July/August 2014.
14. Melamed S, Geffen N, Assia EI. Long term multicenter evaluation of CO2 laser assisted sclerectomy surgery (CLASS) in open angle glaucoma patients. Poster presented at: World Glaucoma Congress; June 2015; Hong Kong.



