
In a perfect world, a cataract could be removed and replaced by an IOL without altering the shape of the cornea. This would greatly improve the procedure’s refractive predictability. Incisions, however, change the shape of the cornea—a phenomenon referred to as surgically induced astigmatism (SIA). The situation could be managed more easily if we ophthalmologists knew in advance the exact effect each incision will have, but SIA is unpredictable. As surgical techniques have improved, incisions have shrunk, and patient expectations have skyrocketed, our appreciation of SIA has grown more quickly than our ability to predict or control it.
We must discard the idea that the cornea simply flattens where an incision is made. SIA is a surprisingly complicated topic.
THE CORNEA IS LIVING TISSUE
It is easy to divide the cornea into two perpendicular meridians, one flatter and the other steeper in curvature. These are the basics of biometry. Many of us were taught that, if an incision is made in the cornea, a flattening effect occurs at that meridian. It is important to appreciate, however, that the cornea is a 3D dome of tissue. The various meridians are related. If one part is flattened, another becomes steeper to compensate.
Our understanding of corneal biomechanics is limited. We cannot predict how a given cornea will respond to an incision. Similarly, difficulties with corneal biomechanics cause trouble predicting the risk of ectasia from keratorefractive procedures and accurately measuring IOP with applanation of the cornea. Thankfully, now we know that creating small incisions minimizes posterior corneal SIA, meaning we only have to worry about one surface of the cornea.1
AS IN REAL ESTATE, IT IS ALL ABOUT LOCATION
The farther an incision is made from the center of the cornea, the smaller the magnitude of the induced change in shape is.2 The human cornea is usually horizontally oval, so temporal limbal incisions are naturally farther from the central cornea and induce less SIA than superior incisions.
Most of us have converted to temporal incisions for their other advantages such as easier access to the eye. Some of us prefer to operate on axis with the intention of making the main incision on the steep axis of the cornea. If a large incision is created, it may induce large, relatively more predictable SIA. With a 2.4-mm or smaller incision, shifting the position of the main wound can potentially cause more harm than good. Moving operating position around the eye creates more variability for the operating team, positioning equipment, and toric alignment systems. It also creates variability in the impact of SIA, making results analysis difficult. Moreover, every incision that is not temporal can increase SIA magnitude simply by being closer to the center of the cornea. In an operation where consistency is key and there is a small margin for error, I strongly recommend to keep your incisions temporal regardless of the steep axis from keratometry.
INCISION SIZE MATTERS
Large incisions (> 6 mm)—as are used in extracapsular cataract surgery—cause flattening in the meridian of the incision and have a predictable effect on the magnitude of change in astigmatism. The effect on SIA of standard 2.4-mm phaco incisions is much harder to anticipate. The magnitude of the change in astigmatism often has a mean value of 0.25 to 0.50 D, but the axis at which it exerts its effect varies widely. Incisions that are as large as 2.2 mm and as small as 1.8 mm have been shown to be astigmatically neutral or produce minimal SIA.3 It is unlikely that these incisions are truly astigmatically neutral, but their impact is minimal compared to measurement accuracy.
There is also some evidence to show that SIA from small incisions may produce asymmetrical changes in the shape of the cornea, resulting in variations in higher-order aberrations such as coma rather than regular astigmatism.4
SIA CAN BE DESCRIBED IN DIFFERENT WAYS
When calculating a toric IOL’s power, SIA is often considered. I am not privy to the inner workings of these formulas, but based on back calculations, many use the SIA value to apply a simple flattening effect at the designated incision location. The magnitude entered into the SIA field therefore has a considerable effect on the astigmatic outcome.
There are various ways of thinking about SIA and considering what value to enter. One is to think of SIA for an individual eye. Pre- and postoperative keratometry readings are measured and compared, and the difference is the SIA for the eye. This can be plotted as a vector, and information on multiple eyes can provide a mean magnitude of SIA. The mean magnitude for a standard 2.4-mm incision is often around 0.30 D. The problem with using this value is that it gives no indication of where that flattening effect will occur. The 0.30 D change in astigmatism could occur perpendicular to where it is expected and double the predicted change. I do not recommend entering this value into a calculator.
The second method of thinking about SIA is to plot the individual change in astigmatism vectors for each eye on a centroid diagram (Figure). The direction and magnitude of average SIA may then be considered. Because of the seemingly random nature of SIA direction, the value of this summated vector mean is usually around 0.10 D. Entering this value in a toric IOL calculator is frequently recommended. The important things to remember are that it is the average magnitude and direction of SIA for a group of eyes and an individual eye may have a higher magnitude of change. The smaller value being entered using the centroid value reduces prediction error in most situations.
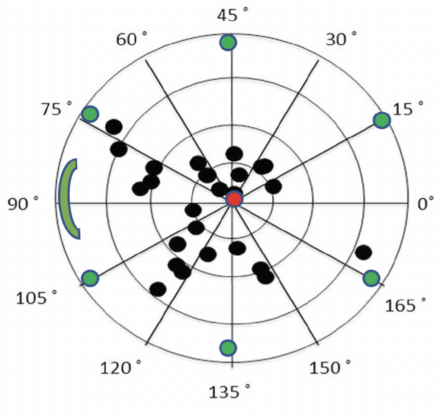
Figure. Centroid plot of SIA for temporal incisions. The black dots indicate individual eyes and location of their maximal flattening effect from Dr. LaHood’s latest (at the time of writing) 25 cataract surgeries with a 2.2-mm incision. The distribution varies greatly in axis and magnitude. The green dots demonstrate that, if each of these represented the SIA from an individual eye, the mean magnitude of SIA would be high but the centroid value (red dot) would be zero because they are equally distributed in direction. This is an extreme example of the different ways of describing SIA.
Lastly, SIA may be thought of as the flattening effect occurring at the meridian of the incision. Because the flattening effect rarely occurs exactly where the incision is made, it is possible to analyze the change in astigmatism and calculate how much of the change occurred at that exact meridian. It is also typically 0.10 D.
My recommendation is to enter zero for the SIA value in a toric IOL calculator because the location of induced astigmatism is unpredictable. If the SIA prediction is probably wrong, my strategy minimizes the impact on the outcome.
CONCLUSION
SIA may be difficult to predict, but its impact can be minimized by making small incisions as far away from the center of the cornea as possible. Factors such as the degree of physical manipulation and operating time also likely play a role in determining SIA magnitude. I invite readers interested in further discussion of SIA to listen to a three-part series on the subject on Ophthalmology Against the Rule, a podcast I cohost.
1. Kane JX, LaHood BR, Goggin M. Analysis of posterior corneal surgically induced astigmatism following cataract surgery with a 1.8-mm temporal clear corneal incision. J Refract Surg. 2023;39(6):381-386.
2. Nikose AS, Saha D, Laddha PM, Patil M. Surgically induced astigmatism after phacoemulsification by temporal clear corneal and superior clear corneal approach: a comparison. Clin Ophthalmol. 2018;12:65-70.
3. He Q, Huang J, Xu Y, Han W. Changes in total, anterior, and posterior corneal surface higher-order aberrations after 1.8 mm incision and 2.8 mm incision cataract surgery. J Cataract Refract Surg. 2019;45(8):1135-1147.
4. Kohnen T, Löffler F, Herzog M, Petermann K, Böhm M. Tomographic analysis of anterior and posterior surgically induced astigmatism after 2.2 mm temporal clear corneal incisions in femtosecond laser-assisted cataract surgery. J Cataract Refract Surg. 2019; 45(11):16021611.



