In 1921, a play by an intellectual named Karel Čapek premiered in Prague that was titled R.U.R., which translates to Rossum’s Universal Robots. The work originated the concept of robots, which was derived from the Czech word robota, meaning forced labor. The play tells a now common story of robotic individuals oppressed into slavery by mankind.1 The future of robots, however, appears to be much brighter than Čapek’s tale.
Robotics has been used to advance minimally invasive techniques in the fields of cardiac surgery, gastroenterology, gynecology, plastic reconstructive surgery, otolaryngology, neurosurgery, vascular surgery, hand surgery, and peripheral nerve surgery.2-5 In oncologic surgery, transoral robotic surgery has been shown to deliver superior outcomes compared to conventional open surgery for head and neck cancers.6 The advances in other fields of surgery notwithstanding, robot-assisted eye surgery has yet to gain traction.
Unlike other surgical specialties, a microscope is required for most procedures in ophthalmology. Ophthalmology is therefore a high-precision microsurgical specialty, often challenging an ophthalmologist’s physical abilities. Additionally, the tissues involved in some ophthalmic surgeries are so delicate that their resistance and the forces needed to manipulate them can be below the human threshold for tactile perception.7 Of note, vitreoretinal surgeons have a physiologic tremor amplitude of 156 µm.8,9 Microstructures such as Schlemm canal and macular holes have diameters of 100 to 200 µm.10,11 Ophthalmic procedures require great skill to perform owing to the physiologic boundaries of the eye and the limitations of spatial resolution and depth perception for adequate tissue plane assessment.12
For some surgeons, procedures such as MIGS pose too high a barrier for entry, prompting them to forego their implementation. Robotics holds promise for ophthalmic surgeons to overcome these barriers.
A FOCUS ON STABILIZATION
Robotics has focused on identifying and neutralizing surgeon tremor.13 In 2020, a group in Japan described an in vitro procedure on porcine eyes with mechanical assistance from a freely movable arm device developed by automobile robotics maker Denso. The Intelligent Arm Support System (iArmS) is essentially a smart armrest that stabilizes the surgeon’s hands during surgery.14
The da Vinci Surgical System (Intuitive Surgical), the first robotic surgical system to be commercialized, was a natural choice for early attempts at robot-assisted ophthalmic surgery. It was used to perform a variety of surface procedures, including penetrating keratoplasty, strabismus surgery, amniotic membrane transplantation, and in vivo pterygium surgery. Cataract surgery was also demonstrated on a synthetic open-sky eye model.15-20
The studies were encouraging but humbling, revealing that the journey to a robotic surgical-assistive device for intraocular surgery would be long. As a result of three specific design limitations, the da Vinci is not suitable for intraocular ophthalmic interventions.
No. 1. The system uses an endoscope for visualization while the surgeon sits outside the sterile field in a cockpit housing the remote controls. The endoscope has been reduced in size to 8 mm, but this is far too large to facilitate intraocular surgery.21
No. 2. The remote positioning of the surgeon from the sterile field and the surgical system’s large footprint prohibit the use of an operating microscope for intraocular visualization.
No. 3. Because it is designed for general surgery, the da Vinci system has large laparoscopic forceps, which do not enable corneal microsurgery and could not be inserted into the eye.22
Given the challenges, the need for an ophthalmic-specific robotic-assistive platform is clear.
THE CURRENT LANDSCAPE
Clinical systems. Multiple platforms for ophthalmic robots are in development. In addition to stabilization of the natural resting hand tremor, design goals include increased precision, automation, better ergonomics, heightened maneuverability, and remote surgery,21 all of which would be relevant not only to experienced ophthalmologists but also to those in training. Additionally, robotic assistance could level the playing field between nonophthalmologists and ophthalmic surgeons in terms of accuracy, stability, and tissue interaction.23
Many robotics programs have emerged from universities (see Recent Ophthalmic Robotics Companies and Programs).24-26 To date, however, the Preceyes Surgical System is the only platform to have received the CE Mark and been used in humans,27 including for macular epiretinal membrane peeling, retinal vein cannulation for central retinal vein occlusion, intravitreal injection, and subretinal gene therapy injection.28,29 Preceyes, acquired by Carl Zeiss Meditec in what is the first ophthalmic robotic merger and acquisition,30 is the only company to develop two ophthalmic surgical platforms—one for retina and one for MIGS (Figure).
Recent Ophthalmic Robotics Companies and Programs
- Acusurgical
- ForSight Robotics
- Horizon Surgical Systems // Spin-off from Intraocular Robotic Interventional and Surgical System // Spin-off from Advanced Robotic Eye Surgery Laboratory at University of California, Los Angeles
- Micron // The Robotics Institute at Carnegie Mellon University
- Mynutia // Spin-off project of the Department of Mechanical Engineering at KU Leuven
- Preceyes in conjunction with the New York Eye and Ear Infirmary of Mount Sinai // Now Carl Zeiss Meditec
- Robot-assisted minimally invasive surgery (RAMIS) // Smartsurg
- Steady-Hand Eye Robot // CiiS Lab at Johns Hopkins University
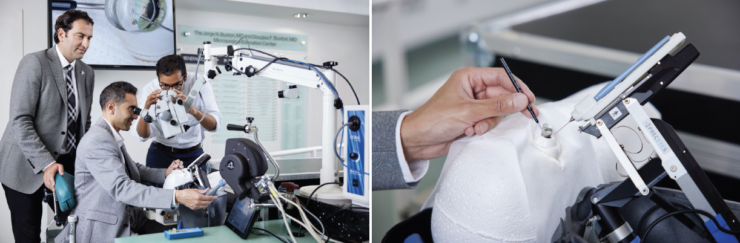
Figure. The Preceyes Robotic System. A module for MIGS was developed in collaboration with the New York Eye and Ear Infirmary of Mount Sinai Innovation Team.
Before the deal with Carl Zeiss Meditec, which could be an indication of what may be a new wave of strategic interest in the space, Preceyes collaborated with New York Eye and Ear Infirmary of Mount Sinai to build the company’s presence in the United States and facilitate its FDA application. Originally, the Preceyes Surgical System was limited to vitreoretinal applications only, but an extended modular application for MIGS was developed in collaboration with New York Eye and Ear Infirmary.31,32 No robotic platform has targeted MIGS explicitly, yet it is the fastest-growing part of the US surgical ophthalmic market.33
Preclinical systems. The Intraocular Robotic Interventional Surgical System (IRISS) was developed at the University of California, Los Angeles, and has been spun off as Horizon Surgical Systems. The goal of this commercial project is to develop a fully automated solution for cataract surgery based on the original IRISS platform. Recent information on Horizon is limited because the company is in stealth mode, according to its website. According to its founder, Jean-Pierre Hubschman, the original IRISS can “react within 20 milliseconds to 30 milliseconds … [and] detects and adjusts immediately to any eye movement.”34
Other stealth preclinical projects have been launched that have received investor backing to the tune of millions of dollars. Such is the case with ForSight Robotics which received $55 million in venture capital funding in 2022.35 The former founders of Intuitive Surgical and Mako Surgical partnered to produce Orym, a platform designed for cataract surgery that incorporates AI and advanced visualization systems. The goal is to help democratize ophthalmic microsurgery by making it more globally accessible.34
CONCLUSION
Developing a robotic surgical assistive system for ophthalmic surgery is challenging, but significant progress has been made during the past 20 years. The limitations of manual surgery and the potential benefits of robotic assistance and automation are driving the field forward. What the future of robotic technology will look like is unclear, but it appears to be less like Karel Čapek’s dystopia and more like human and robotic collaboration.
1. Jordon JM. The Czech play that gave us the word ‘robot.’ The MIT Press Reader. July 29, 2019. Accessed May 9, 2023. https://thereader.mitpress.mit.edu/origin-word-robot-rur
2. Ballantyne GH. Robotic surgery, telerobotic surgery, telepresence, and telementoring. Review of early clinical results. Surg Endosc. 2002;16(10):1389-1402.
3. Hockstein NG, Nolan JP, O’Malley BW, Woo YJ. Robotic microlaryngeal surgery: a technical feasibility study using the daVinci surgical robot and an airway mannequin. Laryngoscope. 2005;115(5):780-785.
4. Broeders IA, Ruurda JP. Robotics in laparoscopic surgery: current status and future perspectives. Scand J Gastroenterol Suppl. 2002;(236):76-80.
5. Nicolau S, Soler L, Mutter D, Marescaux J. Augmented reality in laparoscopic surgical oncology. Surg Oncol. 2011;20(3):189-201.
6. Morisod B, Simon C. Applications de la chirurgie robotique transorale dans les tumeurs de la sphère ORL. Rev Med Suisse. 2013;9(400):1765-1769.
7. Gupta PK, Jensen PS, de Juan Jr E. Surgical forces and tactile perception during retinal microsurgery. In: Taylor C, Colchester ACF, eds. Medical Image Computing and Computer-Assisted Intervention–Miccai ’99: Second International Conference Cambridge UK September 19-22, 1999 Proceedings. Springer; 1999:1218-1225.
8. Riviere CN, Gangloff J, de Mathelin MD. Robotic compensation of biological motion to enhance surgical accuracy. Proc IEEE. 2006;94(9):1705-1716.
9. Peral-Gutierrez F, Liao AL, Riviere CN. Static and dynamic accuracy of vitreoretinal surgeons. Conf Proc IEEE Eng Med Biol Soc. 2004;2734-2737.
10. Shin JY, Chu YK, Hong YT, Kwon OW, Byeon SH. Determination of macular hole size in relation to individual variabilities of fovea morphology. Eye (Lond). 2015;29(8):1051-1059.
11. Irshad FA, Mayfield MS, Zurakowski D, Ayyala RS. Variation in Schlemm’s canal diameter and location by ultrasound biomicroscopy. Ophthalmology. 2010;117(5):916-920.
12. Channa R, Iordachita I, Handa J. Robotic vitreoretinal surgery. Retina. 2017;37(7):1220-1228.
13. Tatinati S, Nazarpour K, Ang WT, Veluvolu K. Multi-dimensional modeling of physiological tremor for active compensation in hand-held surgical robotics. IEEE Transactions on Industrial Electronics. 2017;64(2):1645-1655.
14. Okamura C, Kojima T, Tokiwa S, Hasegawa A, Tanaka Y, Ichikawa K. Microscopic ophthalmic surgery using a freely movable arm support robot: basic experiment and clinical experience. Ophthalmic Res. 2020;63(6):580-587.
15. Bourcier T, Nardin M, Sauer A, et al. Robot-assisted pterygium surgery: feasibility study in a nonliving porcine model. Transl Vis Sci Technol. 2015;4(1):9.
16. Bourcier T, Chammas J, Becmeur PH, et al. Robot-assisted simulated cataract surgery. J Cataract Refract Surg. 2017;43(4):552-557.
17. Chammas J, Sauer A, Pizzuto J, et al. Da Vinci Xi robot–assisted penetrating keratoplasty. Transl Vis Sci Technol. 2017;6(3):21.
18. Bourcier T, Chammas J, Gaucher D, et al. Robot-assisted simulated strabismus surgery. Transl Vis Sci Technol. 2019;8(3):26.
19. Bourcier T, Chammas J, Becmeur PH, et al. Robotically assisted pterygium surgery: first human case. Cornea. 2015;34(10):1329-1330.
20. Bourcier T, Becmeur PH, Mutter D. Robotically assisted amniotic membrane transplant surgery. JAMA Ophthalmol. 2015;133(2):213-214.
21. Bourcier T, Dormegny L, Sauer A, et al. State of the art in robot-assisted eye surgery. Klin Monbl Augenheilkd. 2021;238(12):1290-1293.
22. Bourges JL, Hubschman JP, Burt B, Culjat M, Schwartz SD. Robotic microsurgery: corneal transplantation. Br J Ophthalmol. 2009;93(12):1672-1675.
23. Noda Y, Ida Y, Tanaka S, et al. Impact of robotic assistance on precision of vitreoretinal surgical procedures. PLoS One. 2013;8(1):e54116.
24. Nuzzi R, Brusasco L. State of the art of robotic surgery related to vision: brain and eye applications of newly available devices. Eye Brain. 2018;10:13-24.
25. Gerber MJ, Pettenkofer M, Hubschman JP. Advanced robotic surgical systems in ophthalmology. Eye (Lond). 2020;34(9):1554-1562.
26. Chen CW, Lee YH, Gerber MJ, et al. Intraocular robotic interventional surgical system (IRISS): semi-automated OCT-guided cataract removal. Int J Med Robot. 2018;14(6):e1949.
27. de Smet MD, Naus GJL, Faridpooya K, Mura M. Robotic-assisted surgery in ophthalmology. Curr Opin Ophthalmol. 2018;29(3):248-253.
28. Edwards TL, Xue K, Meenink HCM, et al. First-in-human study of the safety and viability of intraocular robotic surgery. Nat Biomed Eng. 2018;2:649-656.
29. Willekens K, Gijbels A, Smits J, et al. Phase I trial on robot assisted retinal vein cannulation with ocriplasmin infusion for central retinal vein occlusion. Acta Ophthalmol. 2021;99(1):90-96.
30. A new industry partner is a milestone for ophthalmic robotics. Mount Sinai. Accessed May 9, 2023. https://reports.mountsinai.org/article/ophth2022-_4_ophthalmic-robotics
31. Ianchulev T. Robot-Assisted Microinvasive Glaucoma Surgery. Oral presentation at the American Academy of Ophthalmology Spotlight Glaucoma Sub-Specialty Day. November 2021; New Orleans, LA.
32. Kamthan G, Meenink T, Morgan I, et al. Micro-Interventional System for Robot-Assisted Gonioscopic-Surgery. Poster presented at: American Academy of Ophthalmology Annual Meeting; September 2022; Chicago, IL.
33. Hutton D. Iantrek raises $23 million in series B financing for development of MIGS devices in US. Ophthalmology Times. August 31, 2022. Accessed May 9, 2023. https://www.ophthalmologytimes.com/view/iantrek-raises-23-million-in-series-b-financing-for-development-of-migs-devices-in-us
34. ‘Enormous’ potential of robotics opens door to next revolution in eye surgery. Ocular Surgery News. April 25, 2021. Accessed May 9, 2023. https://www.healio.com/news/ophthalmology/20210412/enormous-potential-of-robotics-opens-door-to-next-revolution-in-eye-surgery
35. Hale C. ForSight’s cataract eye surgery robot claims $55M VC round. Fierce Biotech. July 22, 2022. Accessed May 9, 2023. https://www.fiercebiotech.com/medtech/forsights-cataract-eye-surgery-robot-claims-55m-vc-round