
Confusing. This word sums up what many of us think about modern IOL terminology. So many of us have little understanding of so-called premium lenses and their varying mechanisms of action and performance. In this article, working from the concept of first principles I learned during my residency in internal medicine, I hope to provide some clarity on IOL terminology for both ophthalmologists and patients.
POOR TERMINOLOGY
There are myriad examples of poor terminology and abbreviations for IOL designs.
Presbyopia-correcting IOL. Many times, presbyopia-correcting IOL is abbreviated as PCIOL. Those like myself who trained in the 1980s remember that PCIOL is an established abbreviation for a posterior chamber IOL, differentiating this from an anterior chamber IOL.
Not only is the term presbyopia correcting IOL confusing, it is also incorrect. The implants in this category do not correct presbyopia; rather, they increase the range of focus (ROF). These lenses are used for patients who have presbyopia (often combined with another refractive error), but they are also used for patients with cataract to provide optimal vision and increased ROF.
Instead of the term presbyopia-correcting IOL, I suggest the term high-performance IOL, which can be abbreviated as HPIOL.
Extended depth of focus IOL. The acronym EDOF comes from photography, where it refers to the extended depth of field achieved by reducing either the aperture or the magnification of an optical system. EDOF has become a buzzword in IOL design, and manufacturers promote this technology as more forgiving of dysphotopsias with the compromise of a reduced range of focus.
The term EDOF is widely used to categorize lenses that employ a variety of mechanisms to achieve either an increased ROF (IROF) or an extended ROF (EROF) compared with a standard monofocal IOL. The only lenses that truly increase or extend depth of field are small-aperture (ie, pinhole) lenses such as the IC8 (AcuFocus) and XtraFocus Pinhole Implant (Morcher). The remainder are either EROF or IROF implants.
The EDOF designation has been adopted (incorrectly in my view) by the American National Standards Institute (Z80.35-2018) and was published as early as 2015 in the AAO’s Task Force on Consensus on Testing of EDOF Lenses.1 The EDOF lens category is an example of poor terminology that has been promulgated over time. The pretense that these lenses equate to less dysphotoptic phenomenon has prompted other manufacturers to jump on the bandwagon.
MISCONCEPTIONS, CONTROVERSY, AND A PROPOSAL
I am baffled by the excitement surrounding EDOF lenses because it appears to ignore three big misconceptions and one controversy.
• Misconception No. 1. EDOF and IROF lenses are easier for patients to adapt to and more forgiving than other lenses, such as full ROF (FROF) lenses like trifocals.
• Misconception No. 2. Patients are less likely to experience postoperative dysphotopsias with EDOF (IROF) lenses. This is not true. The mechanisms of action of some lenses in this category may result in halos, glare, starbursts, and poor crisp focus.
• Misconception No. 3. EDOF/IROF lenses behave similarly from eye to eye and from patient to patient and is the only variable.
As with all lenses, performance varies among EDOF and IROF lenses, and reliably meeting the expectations of both surgeons and patients can be challenging. The optical performance of an IOL is only one variable in achieving the desired result. Other variables include the following:
- Corneal optics, which depend on shape and level of asphericity and asymmetric aberrations;
- A mean mesopic postoperative pupil size of about 4 mm (personal data);
- Axial length, especially from the posterior nodal point to the fovea (eyes with a short axial length have a more obtuse conoid of Sturm and are less forgiving than long eyes with a thin conoid of Sturm); and
- Capacity for neural adaptation of the recipient.
Controversy. I have observed the debates about classifying some of the new IOL designs as true EDOF, enhanced monofocal, and monofocal plus. All increase ROF to some level, but those that do not meet the American National Standards Institute definition for EDOF must be classified with alternative terminology.
What is obvious is the interplay between three factors:
- No. 1: Lens performance in terms of ROF;
- No. 2: The mechanism of action used to achieve higher performance; and
- No. 3: The propensity for visual disturbances.
A proposal. The American-European Congress of Ophthalmic Surgeons (AECOS) 2020 Summer Series featured a symposium on presbyopia that included discussion about IOL terminology. To prepare for the session, the AECOS program chairs contacted all known manufacturers of high-performance lenses and requested the performance data submitted to regulatory approval authorities and descriptions of the mechanisms of action of their IOLs.
The response from industry was good—although only a few actually provided performance data that had been submitted for CE Mark or US FDA approval. The consensus of the panel discussion was that the term EDOF was ill-suited to this group of lenses for two reasons:
• No. 1. The acronym EDOF typically stands for extended depth of focus, as noted earlier, and should be reserved to describe a lens mechanism of action.
• No. 2. Current IOL terminology should separate lens performance (ie, ROF) from mechanism of action (see the sidebar IOL Categories).
IOL Categories
Category 1
Range of focus (ROF, Figure 1)
- Single focus (ie, monofocal)
- Increased ROF (IROF, Figure 2) Note: the word increased is preferable to extended to avoid confusion with extended depth of focus.
- Full ROF (FROF, Figure 3)
Category 2
Mechanism of action (Figure 4)
- Accommodative
- Small aperture
- Diffractive
- Zonal refractive
- Other
- Combined mechanism
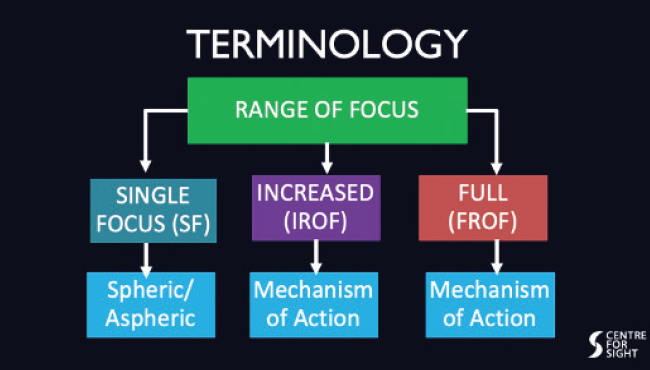
Figure 1. IOL terminology based on the lens’ ROFs.
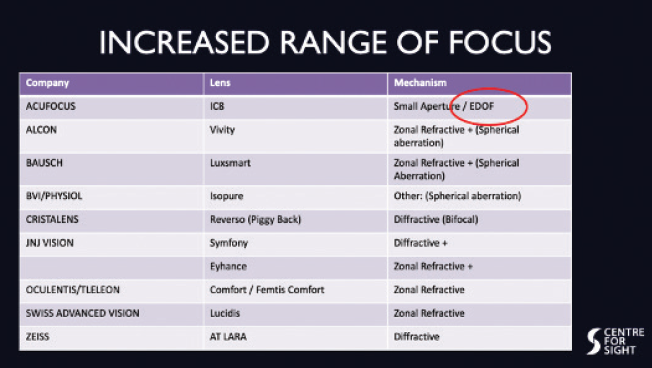

Figure 2. IROF IOLs and their mechanisms of action.
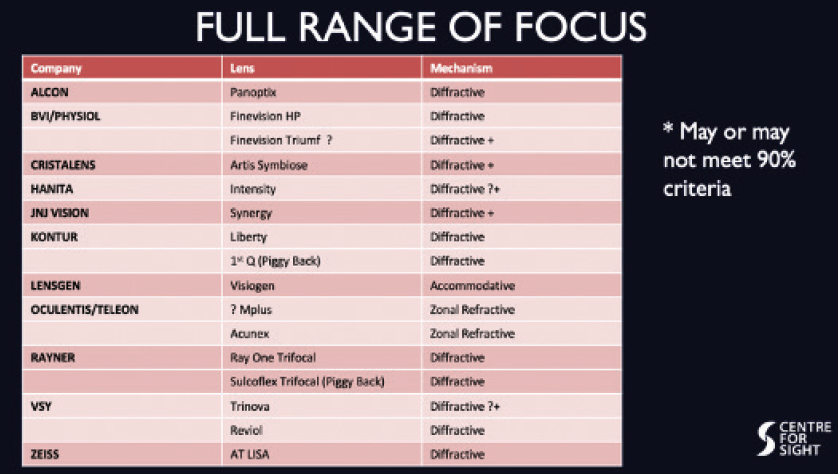

Figure 3. FROF IOLs and their mechanisms of action.

Figure 4. IOL terminology based on mechanism of action.
Based on company responses to the AECOS prompt, we classified the commonly available lenses according to range of performance and mechanism of action (Figures 2 and 3 in the IOL Categories sidebar). As noted earlier, the extent of dysphotopsias after IOL implantation varies considerably based on the IOL’s mechanism of action, level of defocus achieved postoperatively, corneal optics, subjective perception, and neural adaptation.
The terms IROF and FROF may be less confusing than terms such as enhanced monofocal or monofocal plus. They also avoid categorizing IOLs based on a mixture of characteristics related to mechanism of action and performance. The goal of IOL terminology is to simplify what patients should expect in terms of performance and what they might have to contend with in terms of initial side effects (dysphotopsias) based on the mechanism of action.
The incidence and type of postoperative dysphotopsias for each type of lens was not included in AECOS’ proposed categorization of IOLs, but it may be a useful addition to consider.
CONCLUSION
The purpose of categorizing lens terminology is to relay information to patients without confusing them. As things stand, there is considerable confusion even among surgeons. Clear, simple terminology can help ophthalmologists understand what is available to patients, and using this terminology can help patients to make informed decisions. If providers collaborate with the ophthalmic manufacturers and vision scientists who provide IOL technology, I am confident an agreement on language can be reached.
1. Draft consensus statement for comment. American Academy of Ophthalmology. October 7, 2015. Accessed January 22, 2021. Testing_for_EDOF_IOLs_Comment_Document_October_2015.pdf



